There are no standards in this
rapidly changing area, we generally follow the following strategy:
1. for small tumors (T1 or T2N) use standard radiation alone (200cGy) to 66 - 72Gy
2. for patients with larger tumors without node spread (T2-4N0) we generally use
hyperfractionation alone (120 bid to 74-76Gy)
3. for those with T2-T4N1-2 we use chemo-radiation (any of the regimens below)
4. and those with very bulky tumors or neck masses, we use chemotherapy alone first
(neoadjuvant) followed by chemo-radiation.
5. all high risk postop patients should probably get chemoRad (see RTOG 88-24 below and
Bachad)
We have also been treating patients with advanced cancer similar to USF (200cGy to 7000cGy
combined with 5FU/Platinol with a treatment break after 30Gy.) Or similar to UF
(120cGy bid to 7440cGy with PI to 4560 and PII to 6000 / or combined HF with Platinol
30mg/M2/w and stop PI at 4080cGy.) In some of the more frail patients we have used the
Yale Mitomycin protocol (as below.) The current RTOG trials
suggest some options for therapy. RTOG 9501 for postOp XRT compares 60Gy or 60Gy + Platinol (100mg/M2 d1,22,43.) in RTOG 9111 compares induction
5FU/platinol and sequential XRT to chemoRx (concurrent platinol/XRT) in a laryngeal
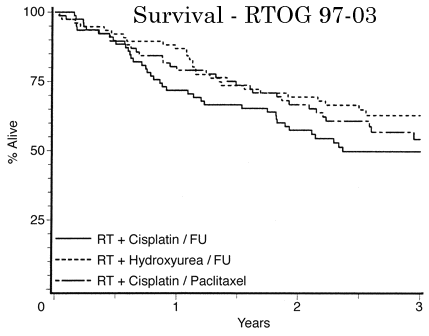
preservation trial. in RTOG 9703 for advanced tumors they use conventional XRT (70Gy) with
three different concurrent chemoRX regimens (platinol/taxol or 5FU/HU or 5FU/platinol.)
and finally RTOG 9914 uses concurrent platinol with AF XRT. For details on the protocols
see RTOG 97-03 or RTOG 99-14. Some of the recent studies
on chemoradiation are noted below
Concomitant weekly cisplatin and altered fractionation radiotherapy in
locally advanced head and neck cancer
Department of Radiation Oncology, University of
Florida College of Medicine, Gainesville, Florida
Both concomitant chemotherapy and altered
fractionation radiotherapy (RT) have been shown to improve outcomes for
patients with locoregionally advanced head and neck squamous cell
carcinomas. However, both strategies also increase acute toxicity, and it is
questionable whether the 2 can be safely combined. Traditional concomitant
chemotherapy regimens include high-dose cisplatin given at 100 mg/m2 every 3
weeks. The authors' purpose was to report efficacy and toxicity after weekly
cisplatin (30 mg/m2/wk) concurrent with altered fractionation RT.
One hundred twenty-one patients with American Joint
Committee on Cancer stages II (3%), III (13%), or IV (84%) squamous cell
carcinomas of the oropharynx (70%), hypopharynx (20%), or larynx (10%) were
treated between 2000 and 2006 at the University of Florida with
hyperfractionated RT (55 patients)
or concomitant boost RT (66 patients) and concomitant cisplatin (30
mg/m2/wk).
Median follow-up was 2.9 years; median follow-up on
survivors was 3.6 years. Seventy-nine percent of patients completed 6 cycles
of chemotherapy; 94% received 7200 centigrays. Seven (6%) patients changed
from cisplatin to carboplatin because of bone marrow toxicity.
Gastrostomy tube feeding was
required in 54% of patients either before (16%) or during RT (38%).
Two (1.6%) patients died from therapy-related complications.
The 5-year outcomes were:
local control, 83%; locoregional control, 79%; distant
metastasis-free survival, 88%;
cause-specific survival, 76%; and overall survival, 59%. Seven (6%)
patients had severe late complications. Three (3%) patients required a
permanent gastrostomy tube.
CONCLUSIONS:
Concomitant weekly cisplatin with altered
fractionation RT is a safe and effective treatment regimen. Cancer 2010. ©
2010 American Cancer Society.
Lancet
2000 Mar 18;355(9208):949-55
Chemotherapy added to locoregional treatment for
head and neck squamous-cell carcinoma: three meta-analyses of updated individual data.
MACH-NC Collaborative Group. Meta-Analysis of Chemotherapy on Head and Neck Cancer.
Pignon JP, Bourhis J, Domenge C, Designe L
Department of Biostatistics and Epidemiology,
Institut Gustav-Roussy, Villejuif, France. jppignon@igr.fr
BWe updated data on all patients in randomised
trials between 1965 and 1993. We included patients with carcinoma of the oropharynx, oral
cavity, larynx, or hypopharynx. The main meta-analysis of 63 trials
(10,741 patients) of locoregional treatment with or without chemotherapy yielded a pooled
hazard ratio of death of 0.90 corresponding to an absolute survival
benefit of 4% at 2 and 5 years in favour of chemotherapy. There was no significant benefit associated with adjuvant or neoadjuvant
chemotherapy. Chemotherapy given concomitantly to radiotherapy gave significant benefits,
but heterogeneity of the results prohibits firm conclusions. Meta-analysis of six trials
(861 patients) comparing neoadjuvant chemotherapy plus radiotherapy with concomitant or
alternating radiochemotherapy yielded a hazard ratio of 0.91 (0.79-1.06) in favour of
concomitant or alternating radiochemotherapy. Three larynx-preservation trials (602
patients) compared radical surgery plus radiotherapy with neoadjuvant chemotherapy plus
radiotherapy in responders or radical surgery and radiotherapy in non-responders. The
hazard ratio of death in the chemotherapy arm as compared with the control arm was 1.19
(0.97-1.46). INTERPRETATION: Because the main meta-analysis showed only a small
significant survival benefit in favour of chemotherapy, the routine use of chemotherapy is
debatable. For larynx preservation, the non-significant negative effect of chemotherapy in
the organ-preservation strategy indicates that this procedure must remain investigational.
Cancer 2000 Feb 15;88(4):876-83
Mature results of a phase III
randomized trial comparing concurrent chemoradiotherapy with radiation therapy alone in
patients with stage III and IV squamous cell carcinoma of the head and neck.
Adelstein DJ, The Cleveland Clinic Foundation,
The current study presents mature results from a
Phase III randomized trial comparing radiation therapy and concurrent chemoradiotherapy in
patients with resectable American Joint Committee on Cancer Stage III and IV disease.
METHODS: One hundred patients were randomized to receive either radiation
therapy alone (Arm A) (at a dose of between 66-72 grays [Gy] at 1.8-2 Gy per day)
and the identical radiation therapy with concurrent chemotherapy
(Arm B) (5-fluorouracil, 1000 mg/m(2)/day, and cisplatin, 20 mg/m(2)/day, both given as
continuous intravenous infusions over 4 days beginning on Days 1 and 22 of the radiation
therapy). Primary site resection was planned for patients with residual or
recurrent local disease. Cervical lymph node dissection was performed for regional
persistent disease or recurrence, or if N2-3 disease was present at the time of
presentation. RESULTS: After completing all therapy including surgery, 82% of the patients in Arm A and 98% of the patients in Arm B had been
rendered disease free.. At a median follow-up of 5 years (range, 3-8 years),
the 5-year Kaplan-Meier projections for overall survival for Arm
A versus Arm B were 48% versus 50% (P = 0.55). Kaplan-Meier projections for the
recurrence free interval were 51% versus 62% (P = 0.04), projections for a distant
metastasis free interval were 75% versus 84% (P = 0. 09), projections for overall survival
with primary site preservation were 34% versus 42% (P = 0.004), and projections for local
control without surgical resection were 45% versus 77% (P < 0.001). Salvage surgery
proved to be successful in 63% and 73%, respectively, of the Arm A and Arm B patients with
primary site failure. Unrelated death while free of disease occurred in 22% and 32%,
respectively, of Arm A and Arm B patients (P = 0.26). CONCLUSIONS: The addition of concurrent chemotherapy to definitive radiation in
patients with resectable Stage III and IV squamous cell carcinoma of the head and neck
improves the likelihood of disease clearance, a recurrence free interval, and primary site
preservation. However, overall survival does not appear to be improved, reflecting both
effective surgical salvage after local recurrence and competing causes of death.
N Engl J Med 1998 Jun 18;338(25):1798-804
Hyperfractionated irradiation
with or without concurrent chemotherapy for locally advanced head and neck cancer.
Brizel. Patients with advanced head and neck
cancer who were treated only with hyperfractionated irradiation received 125 cGy twice
daily, for a total of 7500 cGy. Patients in the combined-treatment group received 125 cGy
twice daily, for a total of 7000 cGy, and five days of treatment with 12 mg of cisplatin per square meter of body-surface area per day and 600 mg
of fluorouracil per square meter per day during weeks 1 and 6
of irradiation. Two cycles of cisplatin and fluorouracil were given to most patients after
the completion of radiotherapy. At three years the rate of overall
survival was 55 percent in the combined-therapy group and 34 percent in the
hyperfractionation group. The relapse-free survival rate was higher in the
combined-treatment group (61 percent vs. 41 percent. The rate of locoregional control of
disease at three years was 70 percent in the combined-treatment group and 44 percent in
the hyperfractionation group.
Int J Radiat Oncol Biol Phys 2000 Apr
1;47(1):49-56
The use of carboplatin and
paclitaxel with daily radiotherapy in patients with locally advanced squamous cell
carcinomas of the head and neck.
Suntharalingam M, Haas ML, Conley BA, Egorin MJ,
Levy S, Sivasailam S, Herman JM, Jacobs MC, Gray WC, Ord RA, Aisner JA, Van Echo DA
Department of Radiation Oncology, Greenebaum
Cancer Center, University of Maryland Medical System,
From 1993-1998, 62 patients with Stage III-IV
SCCHN were treated with 70.2 Gy of RT at 1.8 Gy/fraction/day to
the primary site. Weekly chemotherapy was given during RT consisting of paclitaxel (45 mg/m(2)/wk) and CBDCA (100 mg/m(2)/wk). All
patients presented with locally advanced disease; 77% had T4 disease and 21% had T3
disease. Fifty-eight percent had N2b-N3 disease. A clinical complete response (CR) at the
primary site was obtained in 82%, with a total (primary site and neck) CR rate of 75%. The
median survival for the entire cohort is 33 months. The median survival for patients
who attained a CR is 49 months versus 9 months in those who did not attain a CR (p <
0.0001). The 2- and 3-year overall survival for complete responders are 79% and 61%.
CONCLUSIONS: Weekly carboplatin and paclitaxel given concurrently with definitive
once-daily external beam radiation therapy is well tolerated with over 90% of patients
completing prescribed therapy. An ultimate CR rate of greater
than 70% was obtained, which translated directly into improved survival. With 48% 3-year
overall survival for the entire group, this regimen is an excellent option for
this group of patients with a historically poor prognosis.
J Natl Cancer Inst 1999 Dec 15;91(24):2081-6
Randomized trial of radiation
therapy versus concomitant chemotherapy and radiation therapy for advanced-stage
oropharynx carcinoma.
Calais. A total of 226 patients have been entered
in a phase III multicenter, randomized trial comparing radiotherapy alone (arm A) with
radiotherapy with concomitant chemotherapy (arm B). Radiotherapy was identical in the two
arms, delivering, with conventional fractionation, 70 Gy in 35 fractions. In arm B,
patients received during the period of radiotherapy three cycles of a 4-day regimen
containing carboplatin (70 mg/m(2) per day) and 5-fluorouracil (600 mg/m(2) per day) by continuous infusion. The rate
of grades 3 and 4 mucositis was statistically significantly higher in arm B (71%) than in
arm A (39%). Three-year overall actuarial survival and disease-free
survival rates were, respectively, 51% versus 31% and 42% versus 20%
for patients treated with combined modality versus radiation therapy alone. The
locoregional control rate was improved in arm B (66%) versus arm A (42%).
Radiother Oncol 1997 Apr;43(1):23-8
Neoadjuvant chemotherapy with
cisplatin and 5-fluorouracil in advanced squamous cell carcinoma of the head and neck: a
randomized phase III study.
Lewin Four-hundred sixty-one patients with tumors
in oral cavity, oropharynx, hypopharynx and larynx were randomized to receive either
standard treatment (radiotherapy or radiotherapy followed by surgery) or neoadjuvant
chemotherapy followed by standard treatment. Chemotherapy included three courses of cisplatin 100 mg/m2 i.v. infusion on day 1 followed by 5-fluorouracil 1000 mg/m2 per day continuous i.v. infusion for 120
hours. Radiotherapy 64-70 Gy in 2 Gy per fraction, 5 times/week, was given to patients in
both treatment arms. RESULTS: Response rate was 71% for patients randomized to
chemotherapy-radiotherapy and 66% for patients randomized to standard treatment (not
statistically significant). Residual tumors were excised if possible. After surgery 62% of
the patients randomized to chemotherapy-radiotherapy and 60% of the patients in the
standard treatment group were clinically tumor free. CONCLUSIONS: No
statistically significant benefit in survival was observed for patients treated
with neoadjuvant chemotherapy followed by radiotherapy. Nor was there any impact of
chemotherapy on the number of patients achieving loco-regional tumor control after primary
treatment.
J Natl Cancer Inst 1996 May 1;88(9):583-9
Five-year update of a randomized
trial of alternating radiotherapy and chemotherapy compared with radiotherapy alone in
treatment of unresectable squamous cell carcinoma of the head and neck.
Merlano. One hundred fifty-seven patients with
untreated, unresectable squamous cell carcinoma of the head and neck were randomly
assigned to receive either chemotherapy (four courses of cisplatin
[20 mg/m2] and fluorouracil [200 mg/m2], given daily for 5
consecutive days during weeks 1, 4, 7, and 10) plus radiotherapy (three courses of 20 Gy
each, given in fractions of 2 Gy per day during weeks 2-3, 5-6, and 8-9) or radiotherapy
alone (70 Gy total dose, given in fractions of 2 Gy per day, 5 days per week). Eighty
patients received the combined therapy, and 77 were treated with radiotherapy alone. The
combined treatment was associated with a statistically significant increase in the
frequency of complete response (i.e., the disappearance of clinically detectable disease
for at least 4 weeks) (43% for the combined-treatment group compared with 22% for the
radiotherapy-only group). Five-year estimates of overall survival in the
combined-treatment group compared with the radiotherapy-only group were 24% and
10% respectively. The estimates of progression-free survival
at 5 years in the combined-treatment group compared with the radiotherapy-only group were
21% and 9% respectively.
J Clin Oncol 1997 Jan;15(1):268-76
Chemotherapy as an adjunct to
radiation in the treatment of squamous cell carcinoma of the head and neck: results of the
Yale Mitomycin Randomized Trials.
Haffty. Within each strata, patients were
randomized to receive radiation therapy with or without mitomycin
(trial 1) or mitomycin/dicumarol (trial 2). RESULTS: A total of 203 patients were enrolled
onto both trials, 195 of whom were eligible for analysis. As of September 1995, with a
median follow-up of 138 months, a statistically significant benefit occurred in the
mitomycin arms with respect to cause-specific survival (0.74 v 0.51), local
recurrence-free survival (0.85 v 0.66 ), and local regional recurrence-free survival
(0.76 v 0.54). No statistically significant difference in
overall survival was obtained (0.48 mitomycin arms v 0.42 radiation alone).
J Clin Oncol 1998 Apr;16(4):1318-24
Simultaneous radiochemotherapy
versus radiotherapy alone in advanced head and neck cancer: a randomized multicenter
study.
Wendt . Patients with locoregionally advanced head
and neck cancer were treated either with RT alone (arm A) or simultaneous RT plus CT (RCT;
arm B). RT was identical in both arms and administered in three courses with 13 fractions
of 1.8 Gy each twice daily. During one course, from day 3 to 11, 23.4 Gy was delivered. In
arm B, cisplatin (CDDP) 60 mg/m2, fluorouracil
(5-FU) 350 mg/m2 by intravenous (i.v.) bolus, and leucovorin (LV) 50 mg/m2 by i.v. bolus
were given on day 2, and 5-FU 350 mg/m2/24 hour by continuous infusion and LV 100 mg/m2/24
hours by continuous infusion were given from day 2 to 5. Treatment was repeated on days 22
and 44; a total RT dose of 70.2 Gy was administered. Treatment breaks were scheduled from
days 12 to 21 and days 34 to 43. Acute mucositis grade 3 or 4 was more frequent in arm B
(38%) than in arm A (16%) (P < .001). The 3-year overall survival
rate was 24% in arm A and 48% in arm B. The 3-year locoregional control rate was
17% in arm A and 36% in arm B.
Int J Radiat Oncol Biol Phys 1997 Mar
1;37(4):777-82
Postoperative radiotherapy with concurrent
cisplatin appears to improve locoregional control of advanced, resectable head and neck
cancers: RTOG 88-24.
Al-Sarraf M, Pajak TF, Byhardt RW, Beitler JJ,
Salter MM, Cooper JS
Despite aggressive surgery and postoperative
radiation therapy, only 30% of patients who have advanced, potentially resectable
carcinomas of the head and neck survive for 5 years. In the hope of improving this
situation we studied the effect of postoperative radiotherapy delivered concurrently with
cisplatin. METHODS AND MATERIALS: Patients who had Stage IV tumors
and/or involved surgical margins received 60 Gy in 30 fractions over 6 weeks plus 100
mg/m2 of cisplatin on radiotherapy days 1, 23 and 43. Fifty-two patients
participated in this trial and 51 were evaluated. Forty-three (84%) patients had
pathologic T3 or T4 disease, 43 (84%) had Stage IV disease, and 27 (53%) had
histologically involved surgical margins. RESULTS: Severe and life-threatening toxicities
occurred in 20% and 12% of patients, respectively; the most common drug-related toxicities
were leukopenia, anemia, nausea, and vomiting. Seventeen patients (43%) remain alive with
no evidence of disease. Four patients (8%) died with no evidence of neoplastic disease,
and one patient has died of a second independent malignancy. By
actuarial analysis at 3 years, 48% of patients are alive, 81% have locoregional control of
disease, and 57% are free of distant metastases. CONCLUSIONS: Based on
comparison with similar patients treated in a prior Radiation Therapy Oncology
Group/Intergroup trial (RTOG), we conclude that postoperative radiotherapy with concurrent
cisplatin may improve locoregional control rates and should be prospectively tested.
Int J Radiat Oncol Biol Phys 1996 Dec
1;36(5):999-1004
Combined postoperative radiotherapy and weekly
cisplatin infusion for locally advanced head and neck carcinoma: final report of a
randomized trial.
Bachaud JM, Cohen-Jonathan E, Alzieu C, David JM,
Serrano E, Daly-Schveitzer
PURPOSE: To report the final results of a
prospective randomized trial that aimed to evaluate efficacy and toxicity of concomitant
postoperative radiotherapy and Cisplatin infusion in patients with Stage III or IV
squamous cell carcinoma of the head and neck and histological evidence of extracapsular
spread of tumor in lymph node metastase(s). METHODS AND MATERIALS: Radiotherapy
was delivered using a daily dose of 1.7 Gy for the first 54 Gy and 1.8 to 2 Gy until the
completion of the treatment. Cisplatin 50 mg i.v. with forced hydratation was given or not
every week (i.e., seven to nine cycles) concurrently with radiotherapy. A total of
44 patients were treated by irradiation only (RT group) and 39 by irradiation with
chemotherapy (CM group). RESULTS: The RT group displayed a higher rate of loco-regional
failures as compared to CM group (41 vs. 23%; p = 0.08). The overall survival, the
survival corrected for deaths by intercurrent disease, and the disease-free survival were
better in CM group as compared to RT group with statistically significant
differences. The concomitant use of 50 mg weekly Cisplatin infusion and
postoperative radiation improved loco-regional control and survival. No significant
increase of late radiation complications was observed in the CM group. |