Concurrent Chemotherapy and Radiotherapy for Organ Preservation in Advanced Laryngeal Cancer Arlene A. Forastiere, M.D., NEJM 2003;349:2091 |
|
|
| We randomly assigned
patients with locally advanced cancer of the larynx to one
of three treatments: induction cisplatin plus fluorouracil
followed by radiotherapy, radiotherapy with concurrent
administration of cisplatin, or radiotherapy alone. The primary
end point was preservation of the larynx.
Results A total of 547 patients were randomly assigned to one
of the three study groups. The median follow-up period was 3.8
years. At two years, the proportion of patients who had an intact
larynx after radiotherapy with concurrent cisplatin (88 percent)
differed significantly from the proportions in the groups given
induction chemotherapy followed by radiotherapy (75 percent,
P=0.005) or radiotherapy alone (70 percent, P<0.001). The
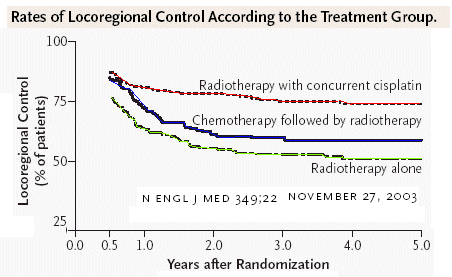
rate of locoregional control was also significantly better with
radiotherapy and concurrent cisplatin (78 percent, vs. 61 percent
with induction cisplatin plus fluorouracil followed by radiotherapy
and 56 percent with radiotherapy alone). Both of the
chemotherapy-based regimens suppressed distant metastases and
resulted in better disease-free survival than radiotherapy
alone. However, overall survival rates were similar in
all three groups. The rate of high-grade toxic effects was
greater with the chemotherapy-based regimens (81 percent with
induction cisplatin plus fluorouracil followed by radiotherapy
and 82 percent with radiotherapy with concurrent cisplatin, vs.
61 percent with radiotherapy alone). The mucosal
toxicity of concurrent radiotherapy and cisplatin was nearly
twice as frequent as the mucosal toxicity of the other two
treatments during radiotherapy. Chemotherapy Induction chemotherapy consisted of cisplatin given intravenously at a dose of 100 mg per square meter of body-surface area on day 1 and fluorouracil given at a dose of 1000 mg per square meter every 24 hours by continuous intravenous infusion for 120 hours, every three weeks for two courses. Patients then underwent evaluation by indirect laryngoscopy and CT imaging of the neck. If these examinations showed a complete or partial response of the primary tumor and no sign of progression in the neck, a third course of cisplatin plus fluorouracil was given, followed by radiotherapy. Patients with a less than partial response of the primary tumor or with progression in the neck underwent laryngectomy followed by adjuvant radiotherapy. Patients assigned to radiotherapy with concurrent cisplatin received intravenous cisplatin at a dose of 100 mg per square meter on days 1, 22, and 43 of radiotherapy.Radiotherapy The dose of radiation and radiotherapy schedule were the same in all three study groups. The dose of radiation to the primary tumor and clinically positive nodes was 70 Gy, given in 35 fractions of 2 Gy each over a seven-week period. The entire neck, including the supraclavicular areas and the posterior neck, was irradiated with a minimum of 50 Gy. The dose to the clinically positive nodes was supplemented with the beams that covered the primary tumor, with electrons, or with tangential anteroposterior beams. The patients assigned to induction chemotherapy followed by radiotherapy who underwent salvage surgery because of a poor response to the chemotherapy received adjuvant radiotherapy (50 to 70 Gy), depending on the status of the margins on pathological review.Conclusions In patients with laryngeal cancer, radiotherapy with concurrent administration of cisplatin is superior to induction chemotherapy followed by radiotherapy or radiotherapy alone for laryngeal preservation and locoregional control.
|