see the whole section on cutaneous lymphoma here
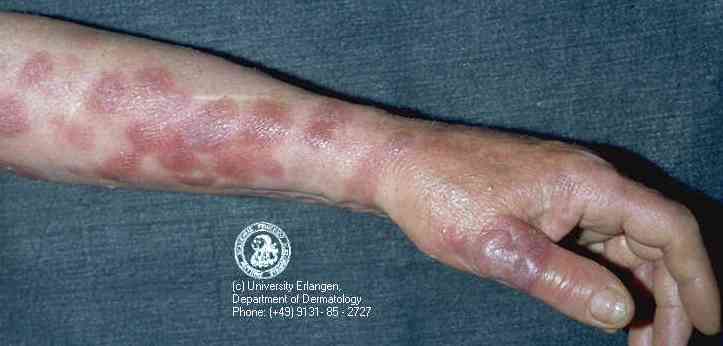

| Mycosis fungoides and the Sezary syndrome is a disease in which certain
cells of the lymph system (called T-lymphocytes) become cancer (malignant) and affect the
skin. Mycosis fungoides and the Sezary syndrome usually develops slowly over many
years. In the early stages, the skin may itch, and dry, dark patches may develop on the
skin. As the disease gets worse, tumors may form on the skin, a condition called mycosis
fungoides. As more and more of the skin becomes involved, the skin may become infected.
The disease can spread to lymph nodes or to other organs in the body, such as the spleen,
lungs, or liver. When large numbers of the tumor cells are found in the blood, the
condition is called the Sezary syndrome. (see pics of advanced disease, pic#1 and pic #2.) If confined to the skin the
patients may respond to either local radiation or treatment of all the skin (total skin
electron beam, see pic.) Radiother Oncol 1999 May;51(2):147-51 Radiotherapy in the management of mycosis fungoides: indications, results, prognosis. Twenty years experience.Kirova YM, Piedbois Y, Haddad E, Levy E, Calitchi E, Marinello G, Le Bourgeois JPDepartment of Cancerology, Henri Mondor University Hospital, Creteil, France. PURPOSE: To determine the role of total skin electron beam therapy (TSEBT) and the prognosis of patients with mycosis fungoides. MATERIALS AND METHODS: From 1978 to 1996, 66 consecutive patients with mycosis fungoides received 30 Gy TSEBT delivered in 12 fractions over 40 days as treatment of their relapsed after topical or/and systemic therapy. All patients were staged as follows: stage A, superficial lesions covering less than 50% of the body surface; stage B, superficial lesions covering more than 50% of the body surface; Stage C. tumors involving the skin, lymph nodes and/or visceral organs. RESULTS: The median age was 50 years (ranging from 13-78 years). There were 39 males and 27 females. The minimum follow-up was 12 months (range 12-192 months). There were 24 (36%) stage A patients, 22 (33%) stage B patients, and 20 (30%) stage C patients. The overall survival at 5 years for our series was as follows: 93% for stage A; 79% for stage B, and 44% for stage C disease (P = 0.002). For the entire cohort, the complete remission rate was 65%, the progression-free survival (PFS) at 5 years and 10 years was 30 and 18% respectively. For the group A, PFS was 62% at 5 years and 46% at 10 years; for group B, PFS was 19% at 5 years. CONCLUSIONS: This study suggests that TSEBT gives good results for relapsed stage A disease. Total skin electron beam therapy combined with local fields irradiation or other local treatment (puvatherapy or topical nitrogen mustard) might further improve permanent complete response for stage B patients. The most advanced stages of mycosis fungoides are not controlled by TSEBT, but the radiation therapy offers good palliation results. Am J Clin Oncol 1992 Apr;15(2):119-24 Total skin electron beam radiation therapy for mycosis fungoides.Reddy S, Parker CM, Shidnia H, Gaffney MG, Blyton BD, Pruner LM, Kalasinski LADepartment of Radiation Oncology, Richard L. Roudebush Veterans Administration Medical Center/Indiana University Medical Center, Indianapolis 46202. Forty-nine patients with biopsy-proven mycosis fungoides, Stages I-IV were treated using total skin electron beam irradiation (TSEBI). Total dose ranged from 600 cGy to 3,200 cGy. To evaluate the dose response relationship, patients were retrospectively divided into two groups. In Group I, 18 patients received a dose of 2,000 cGy or less, and in Group II, 31 patients received more than 2,000 cGy. The overall response rate was 87.7% with a 75.7% complete response and 12.2% partial response. Complete response was higher among patients with early stage disease: (Stage IA 1/1, Stage IB 23/35 (92%), Stage IIA 3/4 (75%), Stage IIB 4/8 (50%), Stage III 3/6 (50%), Stage IVA 1/1, Stage IVB 0/1, and unstaged group 2/3 (66.6%)). Patients treated with a higher total dose had a higher overall 5-year survival rate (Group I 38%, Group II 68%), longer median duration of complete response (Group I, 27 months; Group II, 35.3 months), slightly better complete response rate (72.2% for Group I, 77.4% for Group II), and lower recurrence rate (Group I, 94%; Group II, 83.9%) compared to patients with lower total dose. Complications from TSEBI were minimal. Total skin electron beam irradiation is effective in controlling early stage mycosis fungoides; however, a prospective study to evaluate optimum total dose is needed. Int J Radiat Oncol Biol Phys 1983 Sep;9(9):1279-87 Total skin electron irradiation for mycosis fungoides: failure analysis and prognostic factors.Tadros AA, Tepperman BS, Hryniuk WM, Peters VG, Rosenthal D, Roberts JT, Figueredo ATFrom 1970 to 1980, 106 patients with mycosis fungoides received total skin electron irradiation to full tolerance. The majority received 30 Gy of 3 MeV electrons in 12 treatments over three weeks. Eighty-eight patients had received prior therapy. Fifty patients had cutaneous plaques only (T1-2N0), and 56 had more advanced disease. At five years, actuarial survival is 66.7% and disease-free survival 21.4%. The median time to relapse is 12 months; prolonged survival is seen only with complete response. Compared with more advanced stages, T1-2N0 patients have more frequent complete response (96% vs 71%) and better relapse-free survival at five years (32 vs 7%). Of 14 patients with T2 disease in continuous complete remission for from 45-113 months, only one has relapsed. This suggests that cure is possible in up to 26% of patients with T2 disease who achieve complete response. In advanced stages, complete response is more likely with doses over 25 Gy (80 vs 50%). First recurrences were predominently in sites of previous involvement. Death resulted mainly from extracutaneous dissemination or failure to induce remission. |
![]()