Definitive radiotherapy for
patients with isolated vaginal recurrence of endometrial carcinoma after hysterectomy
Jhingran A, Burke TW, Eifel PJ. International Journal of Radiation
Oncology*Biology*Physics
01 August 2003 (Vol. 56, Issue 5, Pages 1366-1372)
Carcinoma of the endometrium is the most common gynecologic malignancy affecting
women in the Western world. More than 90% of tumors are Stage I, and >80% are cured by
total abdominal hysterectomy and bilateral salpingo-oophorectomy alone. However, in 10–15% of patients, the tumor recurs; about 50% of recurrences are
confined to the pelvis, and about 50% of pelvic recurrences are confined to the vagina.
Postoperative pelvic radiotherapy (RT) reduces the risk of pelvic recurrence in patients
whose tumors have features associated with an intermediate or a high risk of locoregional
recurrence; however, the effect of RT on overall survival (OS) is uncertain. Three
randomized trials have evaluated the benefit of adjuvant pelvic irradiation in patients
with intermediate-risk features. All three demonstrated significant reductions in the
rates of pelvic recurrence with adjuvant RT but failed to show significant improvements in
OS. The authors of these studies suggested that the reason adjuvant RT had no effect on OS
was that successful salvage treatment of vaginal recurrences prevented many patients with
local recurrence from dying of their disease. However, the power of these studies to
reveal clinically relevant effects of adjuvant pelvic RT may have been limited by the
inclusion of many patients with low-risk disease and by follow-up durations too short to
permit detection of any influence of vaginal recurrences on survival.
The purpose of our study was to evaluate the outcome of patients after radical RT for
isolated vaginal recurrences of endometrial carcinoma and to determine the clinical and
pathologic predictors of outcome.
We reviewed the records of 91 patients treated at
our MD Anderson between 1960 and 1997 with radical RT for vaginal recurrence after
definitive surgery for endometrial carcinoma. Thirty-one percent of the patients received
external beam RT (EBRT) alone, 12% received brachytherapy alone, and 57% received a
combination. The median dose of radiation was 75 Gy
(range 34–122). All end points were measured from the time of the first recurrence.
The median duration of follow-up after recurrence was 58 months (range 1–289).
Patients who had combined EBRT and brachytherapy received significantly greater
total doses than did patients treated with either modality alone (90% > 80Gy)
Results
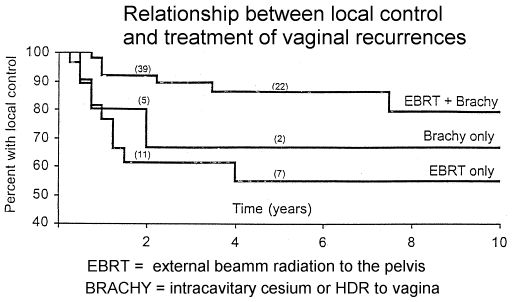
The 2- and 5-year local control (LC) rate and overall survival
rate was 82% and 75% and 69% and 43%, respectively. The median time from
initial diagnosis of endometrial cancer to death from disease was 38 months. On univariate
analysis, a dose to the relapse site of >80 Gy and EBRT plus
brachytherapy vs. single-modality therapy were significant predictors of improved
LC. On multivariate analysis, only the type of treatment correlated significantly with LC
(p = 0.03). On univariate analysis, Grade 1 or 2 vs. Grade 3 tumor and EBRT plus
brachytherapy vs. single-modality therapy were significant predictors of improved overall
survival.
This study describes one of the largest published experiences of patients treated for
isolated vaginal recurrence of endometrial cancer. It confirms that excellent LC rates can
be achieved with RT and suggests that the best results are achieved when high doses of
radiation are given using a combination of EBRT and brachytherapy. However, the results
also suggest that vaginal recurrences are often followed by the development of metastatic
disease and that prevention of vaginal recurrence should be a goal of the initial
treatment of endometrial cancer.
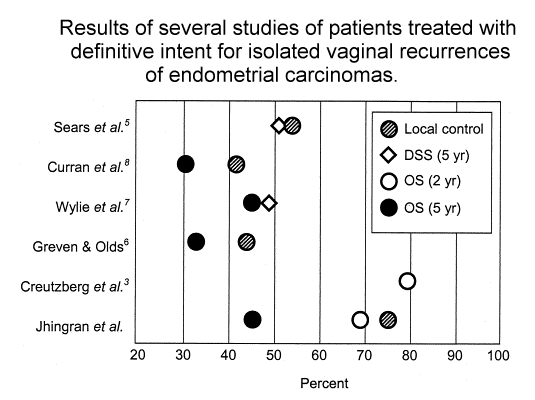
A number of factors have been correlated with LC. Several authors have reported a
relationship between the size of the recurrent tumor and LC
. In a series described by Greven and Olds , 6 of 7 tumors <2 cm in size were
controlled locally compared with only 2 of 10 tumors >2 cm. Wylie et al. reported a
5-year LC rate of 80% in patients with tumors <2 cm compared with 54% in patients with
larger tumors (p = 0.04). In our series, 63% of the patients had tumors <2 cm; however,
LC did not correlate with tumor size and was excellent (about 80%) for patients with small
or large tumors.
Several authors have reported correlations between the location of the vaginal recurrence
and LC. Curran and Aalders found that apical recurrences
had a better response to treatment than more distally located lesions. However,
Phillips and Poulsen found that distally located recurrences had a better outcome, and
other authors did not find any significant correlation between recurrence site and
outcome. These differences may reflect variations in the methods of treatment and in the
types of tumors included in the various studies. For example, in the study by Poulsen ,
patients with lesions in the distal third of the vagina were more frequently treated with
definitive intent than were patients with upper vaginal recurrences (67% vs. 25%). All the
patients in our study were treated with curative intent, and we
found no significant correlation between the site of recurrence in the vagina and LC.
Curran reported that patients who received >60 Gy had significantly better
survival and pelvic control rates than did patients who received lower doses. In another
study, by Wylie, a trend toward better LC was noted in patients who received >80 Gy
compared with those who received <80 Gy . The median radiation dose in our study was 74
Gy; patients who received at least 80 Gy had a significantly
better LC rate than did patients who received <80 Gy (p = 0.04), although
the radiation dose did not correlate with OS. Sears found that patients who had EBRT
followed by a brachytherapy boost had the best overall LC rate , a correlation that was
also significant on multivariate analysis . We also found that patients who received a
combination of EBRT and brachytherapy had better LC and OS rates than did patients who
received a single modality (p = 0.01 for LC and p = 0.02 for OS). In a multivariate
analysis of LC, the type of treatment was the only significant predictor of outcome;
however, the higher doses of radiation delivered to the tumor in patients who received
combined treatment probably contributed to their better LC rate. However, in patients who
had previously been treated with EBRT to the pelvis, brachytherapy alone may be the only
choice, but if the lesion is just outside the previous field, treating with some EBRT
before the brachytherapy procedure, with a small overlap, may be beneficial.
Other factors that have been correlated with outcome after an initial recurrence are the
time to initial recurrence and the grade of the primary lesion. Most
authors have reported a better prognosis for patients who had relatively late recurrences.
However, like several other authors , we did not detect such an association. Some authors
have reported an association between high tumor grade and poor outcome. Hart) reported
that patients with Grade 2–3 tumors had a significantly lower OS rate and poorer LC
than did patients with Grade 1 tumors. In our series, local recurrences were rare
and were unassociated with primary tumor grade; however, patients with Grade 3 primary tumors had a significantly lower survival rate
than did patients with Grade 1 or 2 tumors. This appeared to reflect a higher rate of
distant metastases in patients with Grade 3 tumors.
Despite the excellent LC rate achieved with RT in patients with
recurrent endometrial carcinoma (5-year LC rate 75%), the disease-free survival rate at 5
years was still only 45%. Ultimately, 22 patients in our study (24%) developed
distant metastases despite LC of their disease; 18 of these patients died with
uncontrolled disease. However, in some cases, the time from initial diagnosis of
endometrial cancer to death from disease was quite long. Overall, the median time from
initial diagnosis to death from endometrial cancer was 38 months. This has implications
for studies of adjuvant RT—long follow-up may be necessary to reveal the impact of
prevention of vaginal recurrence on OS. Two recent randomized trials have studied the
effectiveness of RT in patients with a low to intermediate risk of recurrent endometrial
carcinoma. The Post Operative Radiation Therapy in Endometrial Cancer study demonstrated a
reduction in local recurrences from 14% in patients who did not receive pelvic RT to 4% in
patients who did; however, the difference in the OS rate was not statistically
significant. A similar result has been reported for a Gynecologic Oncology Group study of
adjuvant pelvic RT for intermediate-risk endometrial cancer, although the study probably
had inadequate power to detect absolute survival differences of <10–15%. It has
been suggested that in these studies, successful salvage treatment for vaginal recurrences
prevented adjuvant RT from having an impact on OS. Details of the Gynecologic Oncology
Group trial have not yet been published. However, the duration of follow-up in the Post
Operative Radiation Therapy in Endometrial Cancer trial may have been too short to permit
complete evaluation of the impact of vaginal recurrence on outcome. In that study, the
2-year survival rate of 51 patients with vaginal recurrence was 79%. This salvage rate
appeared to be excellent and is similar to our 2-year survival rate of 69%; however, by 5
years, the OS of our patients had fallen to 43%. RT produces excellent LC rates in
patients with isolated vaginal recurrence of endometrial carcinoma (5-year LC rate 75%).
However, because of later distant metastases, only about 45% of patients with isolated
vaginal recurrence survive >5 years. The OS rate is related to the grade of the primary
tumor and the type of treatment used for the recurrent tumor. The LC rate is related to
the dose of radiation applied to the recurrent tumor and the type of treatment used, with
combination treatment (EBRT plus brachytherapy) more effective than either EBRT or
brachytherapy alone. |