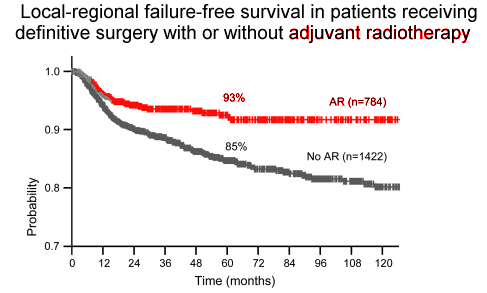
The Role of Adjuvant Radiation in Uterine SarcomasSampath IJROBP 2010;76:728 |
|
|
|
To determine clinical and pathological factors significant for overall survival (OS) and local-regional failure-free survival (LRFFS) in uterine sarcoma as they relate to adjuvant radiotherapy (AR). A retrospective analysis of 3,650 patients with uterine sarcoma was conducted using the National Oncology Database, a proprietary database of aggregated tumor registries owned by Impac Medical Systems (Sunnyvale, CA). Adjuvant radiotherapy was defined as postoperative external beam radiation to the pelvis, with or without brachytherapy. Prognostic factors were identified by multivariate analysis (MVA) using the Cox proportional hazards model. The Kaplan-Meier method was used to estimate survival, with significant differences (p < 0.05) determined using the log-rank test. ResultsThe median follow-up time was 59 months, with a 5-year OS of 37%. Significant prognostic factors for OS were stage, race/ethnicity, grade, age, histology, lymph node status, and surgical treatment. Use of AR was not predictive for OS. For nonmetastatic cancer patients receiving definitive surgery (n = 2,206), the 5-year LRFFS was 87%. In this group, stage, grade, histology, and AR were prognostic for LRFFS (p < 0.05), with AR associated with improved outcome compared with surgery alone (hazard ratio = 0.4, p < 0.001). Patients with carcinosarcoma, endometrial stromal sarcoma, leiomyosarcoma, poorly differentiated tumors, and negative lymph nodes had reduced local-regional failure (LRF) with AR (log-rank, p < 0.05 for all). ConclusionIn the largest retrospective analysis of uterine sarcoma published thus far, AR conferred a 53% reduction in the risk of LRF at 5 years. Use of AR may have broader indications than what are currently accepted in clinical practice. DiscussionThe principal treatment for uterine sarcomas is surgery. The need for additional local therapy is widely debated among gynecologic and radiation oncologists alike. This issue remains controversial because of the paucity of literature providing convincing evidence in favor of or against AR. From a database of 3,650 patents with uterine sarcoma, making this report the largest analysis to our knowledge, we show that AR significantly improves local-regional disease control, with a 53% reduction in the risk of local-regional failure at 5 years compared to surgery alone. Use of AR, was not significantly associated with improved OS. The 5-year OS of 37% is consistent with other large studies, which report 5-year survival rates of 31% to 56%. Significant prognostic variables for OS in our study were stage, race/ethnicity, grade, age, histology, lymph node status, and surgical treatment. Stage is the most consistent prognostic factor for OS, as demonstrated in many series The lack of OS benefit with AR has been described in several retrospective series and one prospective study. This is not surprising given that uterine sarcomas in general demonstrate a high rate of early metastatic spread because of occult distant disease at time of initial diagnosis. Consequently, any potential local benefit gained from AR becomes obscured. However, others suggest that AR significantly improves OS. In a series of 103 patients with various histologies, Ferrer et al. reported a 5-year OS of 73% vs. 37%, in favor of AR. In our study, AR conferred a 53% relative-risk reduction in developing local failures vs. surgery alone. Multiple retrospective series have shown a significant reduction in the rate of local failures with AR. The only Phase III randomized trial to assess the efficacy of adjuvant pelvic radiation therapy (RT) in uterine sarcoma was recently published by the European Organisation for the Research and Treatment of Cancer–Gynecological Cancer Group (EORTC-GCG). Patients with Stage I to II uterine sarcoma were randomized to AR (51 Gy) to the pelvis or observation after total abdominal hysterectomy and bilateral salpingo-oopherectomy. Pelvic and para-aortic lymph node dissections were optional. With a median follow-up of 6 years, AR resulted in a significant reduction in crude local failures in all patients (22% vs. 40%, p = 0.004). Subgroup analysis showed significant local benefit for CS and not for LMS. Statistical analysis of the ESS patients was not possible because of the small sample size. Subgroup analysis of our data showed AR to have a benefit for CS, LMS, and ESS. The benefit seen with AR for CS has been echoed in several retrospective series. Based on its higher rate of isolated local failures and propensity for nodal involvement compared with LMS, CS can be viewed as a poorly differentiated form of endometrial cancer. The EORTC study reported higher rates of isolated distant metastases in the AR arm (25% vs. 10%) and concluded that AR should be reserved for local relapse. When looking at the CS group alone, the AR arm had a overall distant relapse rate of 35%, vs. 29% in the observation group (a difference of three patients), while significantly reducing local failures from 47% to 24% (p < 0.05). Based on our study and the EORTC findings, a strong argument can be made for recommending AR in early-stage CS patients. Our results indicate that AR significantly reduced local failures in LMS. The benefit was small, but was significant statistically because of the large sample size. Use of AR was more likely in patients at highest risk for local recurrence, biasing results against the radiotherapy group. Even with adverse selection, we were able to detect a significant local control benefit with AR. The EORTC-GCG trial showed similar local failure rates (20% vs. 24%) between the AR and observation arms in LMS. Interestingly, in that trial, AR reduced the rate of isolated local failures from 14% to 2%. This is in agreement with our results, in which AR lowered the local failure rate from 16% to 2% at 5 years. The EORTC authors strongly advocated against AR in LMS, citing the higher rate of distant metastases in the AR (54%) vs. the observation arm (33%) of the LMS group. In that study, there was a large discrepancy in the number of isolated distant failures between the AR arm (18 of 50 patients, 36%) vs. the observation arm (7 of 49 patients, 14%). The difference reflects the large heterogeneity of disease burden among LMS patients that is not captured in the current FIGO staging system, where any uterine-confined tumor is considered Stage I regardless of size. It is accepted that larger LMS tumors have a higher metastatic potential. In the EORTC trial, more large tumors may have been disproportionately assigned to the AR arm. As each arm had only 50 patients, an imbalance in tumor characteristics could have a more pronounced effect on outcome, which may explain the higher rate of distant failure found in the AR group. Stratifying patients on the basis of tumor volume rather than stage may better identify those LMS patients who would benefit the most from AR. Our data and the EORTC findings both suggest that there exists a subset of LMS patients (perhaps with small volume disease) who develop isolated local relapse. This would be the group for which AR would have a significant impact on outcome. Unfortunately, our database did not have information on tumor volume. For patients with distant disease, quality of life can be improved with AR. Local-regional disease control in the pelvis with AR can prevent intractable pain, infections, and bleeding associated with pelvic failures. Novel chemotherapy combinations, such as gemcitabine and docetaxel, are demonstrating a 35% response rate as first-line therapy in the metastatic setting. As distant relapse rates improve in LMS, optimizing local control with AR may become a higher priority in the future. There are several studies suggesting that AR does not improve local control. A series of 155 cases of uterine sarcomas from Sweden showed a local-regional relapse-free survival of 75% for the AR group, vs. 83% for patients receiving surgery alone (4). Patient selection likely contributed this result, with more advanced cases requiring AR, resulting in poorer outcomes. Tinkler et al., in a retrospective review of 82 cases from Edinburgh, found no benefit with AR for local tumor control. Over the last 20 years, the Gynecology Oncology Group (GOG) conducted several prospective studies in which AR either was not randomized or was not compared with a surgery-alone control arm. Overall, these trials suggest that AR can lead to a reduction in local failures. GOG 20 was a Phase III trial that randomized 225 women with Stage I/ II uterine sarcoma to adriamycin vs. no additional therapy after definitive surgery. An unplanned subgroup analysis of the data showed a significant decrease in pelvic failures from 54% to 23% in favor of patients receiving AR. The GOG surgical-pathologic study by Major et al. included patients with CS and LMS. A total of 453 patients with clinical Stage I/II disease received a TAH/BSO, with 95% receiving full nodal staging. In the CS group, AR decreased the 3-year pelvic failure rate from 24% to 17%. In the LMS group, eight of 46 patients (17%) who had surgery alone had pelvic failure, whereas no local failures were observed in the 13 patients who had AR. In GOG 150, Stage I–IV CS patients were randomized to whole-abdomen RT or adjuvant chemotherapy after definitive surgery. Analysis of initial sites of failure showed a lower rate of vaginal failures in the radiation arm vs. the chemotherapy arm (3.8% vs. 9.9%), which was not statistically significant because of the small patient numbers. There was no difference in the rates of isolated pelvic failures (13%). However, pelvic radiation was shown to be effective, with a lower combined pelvic and vaginal failure rate at 5 years (17%) when compared with 5-year local-regional failure data from subgroups in other trials treated with surgery alone, which range from 24% to 48%. Abdominal radiation was used sparsely in our patients and therefore further analysis of its efficacy was not performed. We showed on MVA that grade, stage, AR, histology, and nodal status significantly influenced LRFFS. Major et al. reported that LN status, histology, and grade were also significant factors for local failure, in addition to the presence of adnexal disease. In an MVA for pelvic disease control in 273 patients who received surgery, Callister et al. showed the following variables to be significant and to carry a worse prognosis: peritoneal disease (relative risk [RR] = 6.0), prior pelvic RT (RR = 2.0), and surgery without RT (RR = 1.8) . Peritoneal or adnexal disease and history of prior RT were not specifically coded in our database, and therefore we were unable to include them in our MVA. Both LMS and ESS were found in our MVA to be associated with superior local disease control compared with CS. In the EORTC-GCG study, the LMS patients had a lower local recurrence rate (22/99, 22%) compared with the CS patients (33/91, 36%). It is recognized that LMS has a high propensity for early hematogenous spread. As early metastatic failures were recorded for the LMS patients in our database, all subsequent local failures may not have been detected, possibly leading to underreporting. The overall local failure rate (15% at 5 years) parallels those in four other retrospective series with more than 100 patients, which report 5-year local failure rates of 12% to 17% However, other large series report 5-year local failure rates of 38% to 46%. The variability in local surveillance protocols among institutions could be a contributing factor to the differences in reported local failures. The relationship between lymph node status, histology, and AR, and their impact on LRFFS has not been formally studied in the literature. In the CS cohort, those with negative lymph nodes had significantly less local failures with AR. These patients had a higher propensity for experiencing local failure in the primary site because of the low likelihood of occult extrapelvic or “skip” nodal metastases in the context of negative pathologic pelvic nodes, paralleling endometrial cancer. Because of the small number of CS patients with positive lymph nodes, analysis was limited. Information on lymph node status was not available in a large number of patients because of the unknown overall stage. In these patients, we did not know whether LND was performed, and therefore, the impact of AR could not be assessed. In the EORTC-GCG trial, only 25% received LND; outcomes were not stratified by extent of surgery, and sites of local failure (nodal vs. soft tissues) were also not reported. Therefore, the question remains unanswered whether AR can specifically benefit those patients who do not undergo LND. Future studies that specify local failure by site (pelvic soft tissues vs. nodes) as a function of type of surgery will be helpful in further understanding how AR can benefit women with localized uterine sarcomas who receive a complete primary resection. |