| Over the years, treatment for
primary testicular lymphoma has been variable. Treatment using radiation
therapy alone provides suboptimal disease control, even for patients with
clinically stage I disease. Chemotherapy without anthracyclines was
shown to produce inferior results compared with regimens with anthracyclines.
Thus, chemotherapy with anthracycline-containing regimens is the recommended
therapy after orchiectomy. However, despite the administration of aggressive chemotherapy
regimens, prognosis is often still poor, even in localized disease, with
the 2-year relapse rate exceeding 50% in most series.
Patterns of Outcome and Prognostic Factors in
Primary Large-Cell Lymphoma of the Testis in a Survey by the International Extranodal
Lymphoma Study Group
Journal of Clinical Oncology , Vol 21,
Issue 1 (January), 2003: 20-27
To determine clinical features and patterns of
outcome of primary testicular diffuse large B-cell lymphomas (DLCL). Patients
and Methods: A retrospective international survey of 373 patients with
primary testicular DLCL.
Results: Most patients presented
with localized disease (stage I to II), and the median age at diagnosis was 66
years (range, 19 to 91 years). Anthracycline-based chemotherapy was
administered to 255 patients (68%), and prophylactic intrathecal chemotherapy
was given to 68 patients (18%); 133 patients (36%) received prophylactic
scrotal radiotherapy. Median overall survival was 4.8 years, and median
progression-free survival was 4 years. The survival curves showed no clear
evidence of a substantial proportion of cured patients. A favorable
international prognostic index score (IPI), no B-symptoms, the use of
anthracyclines, and prophylactic scrotal radiotherapy were significantly
associated with longer survival at multivariate analysis. However, even for
patients with stage I disease and good-risk IPI, the outcome seems worse than
what was reported for DLCL at other sites. At a median follow-up of 7.6 years,
195 patients (52%) had relapsed. Extranodal recurrence was reported in 140
cases. Relapses in CNS were detected in 56 patients (15%) up to 10 years after
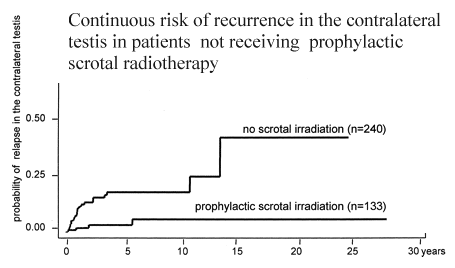
presentation. A continuous risk of recurrence in the contralateral testis
was seen in patients not receiving scrotal radiotherapy. Because
patients were treated according to the current policy of each institution
at the time of diagnosis, there is a wide range of radiotherapy doses (from 18
to 50 Gy) and fields (from scrotal only to a variety of extended fields with or
without contralateral testis) among the 196 patients who received radiotherapy.
Conclusion: Testicular DLCL is
characterized by a particularly high risk of extranodal relapse even in cases
with localized disease at diagnosis. Anthracycline-based
chemotherapy, CNS prophylaxis, and contralateral testicular irradiation seem to
improve the outcome. Their efficacy is under evaluation in a prospective
clinical trial.
Before the widespread use of anthracycline
chemotherapy, patients with stage I and II testis lymphomas were managed mainly
with postorchiectomy radiotherapy to the para-aortic and pelvic lymph nodes.
At present, radiotherapy to the retroperitoneal nodes has largely been
abandoned in stage I patients, but it is generally given to stage II patients
as part of the combined-modality approach recommended in stage II DLCL
presenting in other sites. Unfortunately, the wide variability of doses and fields in our
retrospective analysis prevented a reliable study of the impact of
retroperitoneal radiotherapy in localized testis lymphomas, although the
prognostic impact of this strategy seems to be dose-dependent.
A substantial rate of failure in the contralateral
testis has been reported in the literature, and it has been confirmed in our
cases where continuous high risk of recurrence in the contralateral testis is
documented in patients not receiving prophylactic scrotal radiotherapy . Our
data confirm that low-dose radiotherapy to the contralateral testis, which has
been recommended by some authors for all patients with primary testis
lymphoma,could reduce the risk of failure at this site.
Distant extranodal failures, especially in the
CNS, remain a major problem, even in patients who receive a full course of
doxorubicin-based chemotherapy. The issue of optimal treatment of
patients at the time of isolated CNS relapses is unresolved. Whole-brain
radiotherapy is most often used; however, this treatment has substantial
potential neurotoxicity, especially in the elderly. A recent report indicates
that high-dose intravenous methotrexate alone might be a feasible and effective
alternative to whole-brain radiotherapy. The high rate of CNS progression
observed in historical series has led to a recommendation for routine CNS prophylaxis
with at least intrathecal chemotherapy.The value of intrathecal chemotherapy, introduced
as a prophylactic measure in the 1990s, is still controversial because CNS
failures occur more frequently in brain parenchyma than in meninges, and
CNS relapses have been observed also in patients who received intrathecal
chemotherapy. A clear propensity for parenchymal involvement is confirmed in
our study and is in marked contrast to primary nodal DLCL, where the CNS
relapse rate is below 5% and the leptomeninges are the dominant site of
involvement.In our series, intrathecal chemotherapy was associated with an
improved PFS; however, its direct effect on preventing CNS relapses was not
statistically significant, possibly because of the low number of patients who
received such treatment (80% of CNS relapses did not receive any intrathecal
prophylaxis).
The use of high-dose methotrexate to deliver
parenchymal CNS prophylaxis has been shown to be effective among patients with
primary nodal lymphomas but is not always practical or
feasible in elderly patients, and even the delivery of standard intrathecal
chemotherapy is often problematic. In this series, only 29 patients (8%)
received high-dose intravenous methotrexate as CNS prophylaxis, apparently with
no evidence of any benefit in either reducing CNS relapses or prolonging
survival; but again, the small number of treated cases does not allow any
conclusions to be drawn. On the contrary, the small subset of patients who
received aggressive systemic chemotherapy and complete prophylaxis (intrathecal
chemotherapy and scrotal irradiation) showed a significantly better
outcome, with a 3-year actuarial OS rate of 88%. However, their median
follow-up is short, a possible selection bias cannot be ruled out, and the
efficacy of this policy has yet to be validated in prospective clinical trials.
In conclusion, this retrospective IELSG survey
represents the largest body of information on outcomes of patients with testis
lymphoma to date. It confirms the findings of smaller studies and
provides interesting data concerning the best treatment strategy, but because
of its retrospective nature, it does not provide a definitive answer as to the
optimal approach to this disease.
The management of patients with testicular
lymphoma presents several challenges. Because of the poor prognosis, an
aggressive treatment approach is warranted. However, testicular lymphoma is
predominantly a disease of older men who often have limited ability to tolerate
aggressive treatment. Improved understanding of the genetic and molecular
characteristics of testicular lymphoma may help in the future to identify
patients at risk of CNS failure and to tailor the treatment to the individual
patient.
The rarity of the disease makes randomized trials
virtually impossible. Hence, an international collaboration is crucial to
properly address the management of testicular lymphoma. On the basis of the
results of this study, an international prospective trial has been launched by
the IELSG to assess the feasibility and efficacy of prophylactic radiotherapy
to the contralateral testis and intrathecal methotrexate in addition to
rituximab plus CHOP chemotherapy. This study should test the results of this
retrospective analysis and can provide further evidence to support the use of
systemic chemotherapy and complete prophylaxis (intrathecal chemotherapy and
scrotal irradiation), thus helping to define some standard guidelines for the
management of testicular DLCL. We are aware that the potential benefit of
rituximab for a lymphoma arising in immune privileged sites remains
questionable (despite data suggesting its crossing of the blood-brain barrier,
it does not seem to penetrate into CNS well when administered intravenously,
and its intrathecal administration is poorly studied). However, the association
of rituximab plus CHOP has been shown to be significantly better than CHOP
alone,and it is considered the standard treatment of DLCL at any site in
several institutions. Given the observed propensity for parenchymal involvement
of CNS relapses, other regimens, capable of circumventing the blood-brain
barrier, might be more appropriate in view of the CNS penetration of
methotrexate and cytarabine, but it may be difficult to test an aggressive
regimen in a large multicentric study of mainly elderly patients.
Outcome and patterns of failure in
testicular lymphoma: a multicenter rare cancer network study .
Zouhair.IJROBP 2002;52:652
Primary extranodal lymphoma
of the testis is a lethal disease, second only to primary brain lymphoma; median survival
is 12 to 24 months. It accounts for approximately 1% of non-Hodgkin’s lymphomas, 4%
of all extranodal non-Hodgkin’s lymphomas, and 5% of all testicular malignancies . Primary testicular lymphoma is essentially an intermediate or
high-grade lymphoma, and diffuse large-cell type is the most common . In contrast to other
testicular malignancies, primary testicular lymphoma occurs mostly in patients older than
50 years of age. After adequate locoregional and systemic treatment, central nervous
system (CNS) remains the most frequent site of recurrence (up to 30%). Therefore,
prophylactic intrathecal (IT) chemotherapy (CT) combined with systemic treatment has been
introduced to improve outcome
To assess the outcome and patterns of failure in
patients with testicular lymphoma treated by chemotherapy (CT) and/or radiation therapy
(RT). Data from a series of 36 adult patients with Ann Arbor Stage I ( n = 21),
II ( n = 9), III ( n = 3), or IV ( n = 3) primary testicular
lymphoma, consecutively treated between 1980 and 1999, were collected in a retrospective
multicenter study by the Rare Cancer Network. Median age was 64 years (range: 21–91
years). Most patients ( n = 29) had CT, consisting in most cases of
cyclophosphamide, doxorubicin, vincristine, and prednisolone (CHOP) with ( n =
17) or without intrathecal CT. External RT was delivered to scrotum alone ( n =
12) or testicular, iliac, and para-aortic regions ( n = 8). The median RT dose
was 31 Gy (range: 20–44 Gy) in a median of 17 fractions (10–24), using a
median of 1.8 Gy (range: 1.5–2.5 Gy) per fraction. The median follow-up period was 42
months (range: 6–138 months).
External radiation therapy was given to 22 (61%)
patients . Irradiation volume consisted of the scrotum alone in 13 patients
(bilateral in all) and the scrotal, iliac, and para-aortic regions in 9 patients (4
Stage I, 5 Stage II). Megavoltage photons and/or electrons were used in all patients. . A
median total dose of 31.0 Gy (range: 20.0–44.0 Gy) was given in a median of 1.8
Gy/fraction (range: 1.5–2.5 Gy/fraction) over a median period of 26 days (range:
12–42 days). One patient received prophylactic whole-brain radiotherapy to a total
dose of 12 Gy in 6 fractions.
 After a median period of 11 months (range: 1–76
months), 14 patients presented lymphoma progression, mostly in the central nervous
system (CNS) ( n = 8). Among the 17 patients who received intrathecal CT, 4
had a CNS relapse ( p = NS). No testicular, iliac, or para-aortic relapse was
observed in patients receiving RT to these regions. The 5-year overall,
lymphoma-specific, and disease-free survival was 47%, 66%, and 43%, respectively. In
univariate analyses, statistically significant factors favorably influencing the outcome
were early-stage and combined modality treatment. Neither RT technique nor total dose
influenced the outcome. Multivariate analysis revealed that the most favorable independent
factors predicting the outcome were younger age, early-stage disease, and combined
modality treatment. After a median period of 11 months (range: 1–76
months), 14 patients presented lymphoma progression, mostly in the central nervous
system (CNS) ( n = 8). Among the 17 patients who received intrathecal CT, 4
had a CNS relapse ( p = NS). No testicular, iliac, or para-aortic relapse was
observed in patients receiving RT to these regions. The 5-year overall,
lymphoma-specific, and disease-free survival was 47%, 66%, and 43%, respectively. In
univariate analyses, statistically significant factors favorably influencing the outcome
were early-stage and combined modality treatment. Neither RT technique nor total dose
influenced the outcome. Multivariate analysis revealed that the most favorable independent
factors predicting the outcome were younger age, early-stage disease, and combined
modality treatment.
 In this multicenter retrospective study, CNS was found
to be the principal site of relapse, and no extra-CNS lymphoma progression was observed in
the irradiated volumes. More effective CNS prophylaxis, including combined modalities,
should be prospectively explored in this uncommon site of extranodal lymphoma. In this multicenter retrospective study, CNS was found
to be the principal site of relapse, and no extra-CNS lymphoma progression was observed in
the irradiated volumes. More effective CNS prophylaxis, including combined modalities,
should be prospectively explored in this uncommon site of extranodal lymphoma.
|
|
Primary testicular non-Hodgkin’s lymphoma is an
uncommon disease, and its treatment is not standardized. Orchidectomy is the standard
initial treatment of suspected primary tumors of the testis .
Lymphomas are the most frequent cause of testicular tumors in men more than 50 years of
age . In our series, the median age was 64 years (range: 21–91 years).
The prognosis of testicular
lymphoma is relatively poor compared to other nodal or extranodal lymphomas . Because of
the rarity of this disease, the majority of the patients reported in retrospective series
were probably not staged completely as recommended, which may reflect the poor
outcome . Even in our series, a full staging workup could not be completed in 50% of
patients.
The overall poor outcome of
this disease has been linked to various prognostic factors, including advanced age at
presentation , constitutional symptoms
, bulky primary tumor , spermatic cord involvement , presence of vascular invasion
, and degree of sclerosis . The most important predictive
factors are the stage and pathologic grading . Patients with Stage IE and IIE
disease have better outcome than those with advanced-stage disease .
Among the various prognostic
factors studied in our series, i.e., age, stage, spermatic cord infiltration, grade, LDH,
ß-2-microglobulin, and type of treatment, only younger age and early stage were
independent prognostic factors influencing favorably the overall and disease-free
survival. These two factors are part of the International Prognostic Index .
The universally accepted
treatment modality for Stage I and II aggressive nodal lymphoma is combined chemotherapy
and radiation therapy However, an optimal treatment approach has not been defined
for extranodal lymphomas. Neither have randomized studies been performed evaluating the
superiority of combined modality treatment to RT or CT alone, especially in testicular
lymphoma. Connors , in their study of 15 patients with Stage I and II disease given
combined modality treatment, observed 93% actuarial relapse-free survival. However, in a
retrospective study by Fonseca that included 62 patients, no beneficial effect of combined
treatment compared to single modality was observed. In their study, only 10 patients,
including 3 with Stage I disease, received combined modality treatment. Moreover, only 4
patients received IT-CT, and 2 of these already had leptomeningeal involvement at
diagnosis. It is, therefore, difficult to draw a conclusion about the inefficiency of
combined treatment.
In the present series,
univariate analyses revealed that patients treated with combined CT and RT did better than
those treated with CT or RT alone in terms of overall, disease-free, and lymphoma-specific
survival. Moreover, multivariate analysis revealed that combined treatment was an
independent factor for lymphoma-specific survival.
The patterns of failure after
the initial treatment of testicular lymphoma include mainly the CNS, contralateral
testis, Waldeyer’s ring, skin, pleura, lung, liver, spleen, bone, and bone marrow
. Lymphoma progression is rarely observed in irradiated volumes . CNS relapse, both as
intracerebral and/or leptomeningeal, was reported by many authors, with an incidence of up
to 30% . IT-CT is indicated in patients with proven leptomeningeal
involvement . The role of CNS prophylaxis in patients without CNS involvement remains to
be proven, and its beneficial effect is still controversial . It may be important to distinguish
intraparenchymal failures from the leptomeningeal ones, which are rarely detailed in the
literature.
In our series, no patients
relapsed in irradiated volumes. The majority of relapses (12 out of 14) were in extranodal
sites. Eight (22%) patients had CNS relapse: 4 intracerebral and 4 leptomeningeal. Half (
n = 4) of these relapses were at the unique site of lymphoma progression. IT-CT did
not significantly prevent CNS relapse: Of the 17 patients who received prophylactic IT-CT,
4 patients relapsed (intracerebral in 2, meningeal in 2), whereas of the 19 patients who
did not have prophylactic IT-CT, a total of 4 also relapsed (intracerebral in 2, meningeal
in 2).
In this retrospective
multicentric study including patients with primary testicular lymphoma, we conclude that
CNS is the principal site of relapse, and no lymphoma progression was observed in
irradiated volumes. Patients treated with combined modality, including chemotherapy and
radiation therapy, did better than those treated with a single modality. On the other
hand, to prevent intraparenchymal failure, more effective CNS
prophylaxis, such as low-dose whole-brain irradiation or high-dose methotrexate, must be
prospectively explored. |