| RESULTS:
Motor function
improved in 40% (n = 207), remained stable in
54% (n = 279), and deteriorated in 7% (n = 35) of
patients. Fifty-eight (54%) of 107
nonambulatory patients became ambulatory, and
388 (94%) of 414 ambulatory patients remained
ambulatory. Improved functional
outcome was significantly associated with
tumor type and slower development of motor deficits (>
14 days). Local control at 1, 2, and 3 years
was 92%, 88%, and 78%, respectively. Improved
local control was significantly associated
with long-course radiotherapy.
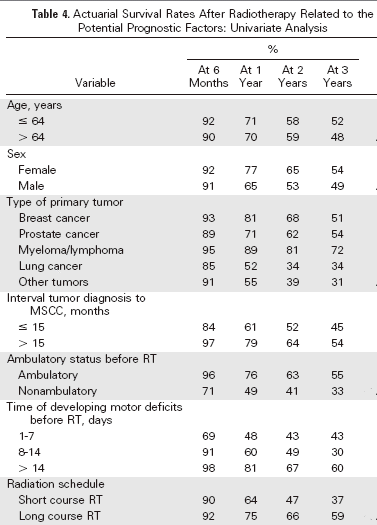
Survival at 1,
2, and 3 years was 71%, 58%, and 50%,
respectively. Better survival was
significantly associated with tumor type, ambulatory
status, slower development of motor deficits,
and long-course radiotherapy. Patients who
developed motor deficits slowly (onset > 14
days before initiating treatment) were further analyzed.
In this subgroup, the best results were
observed for myeloma/lymphoma and breast
cancer patients. No patient had progression of motor
deficits. One hundred percent (myeloma/lymphoma)
and 99% (breast cancer) of patients were
ambulatory after radiotherapy. One-year local
control was 100% and 98%, 1-year survival was 94% and
89%.
CONCLUSION: Given the
limitations of a retrospective review, improved outcome
of patients with oligometastatic MSCC was
associated with myeloma/lymphoma and breast
cancer, slower development of motor deficits, and
a more prolonged course of radiation.
|
 |
