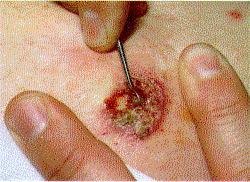
 Treatment Basal Cell Carcinoma / Electrodesiccation
and curettage. Habif: Clinical Dermatology, 3rd ed., Copyright ©
1996 Mosby-Year Book, Inc.
Treatment Basal Cell Carcinoma / Electrodesiccation
and curettage. Habif: Clinical Dermatology, 3rd ed., Copyright ©
1996 Mosby-Year Book, Inc.TECHNIQUE--ELECTRODESICCATION AND CURETTAGE OF BASAL CELL CARCINOMA The technique for electrodesiccation and curettage of nodular basal cell carcinoma (BCC) is as follows: Local anesthesia is induced with lidocaine and epinephrine. The surrounding tissue is supported with the finger, and the soft, friable tumor is curretted until firm dermis is reached. The soft-textured tumor offers little resistance to the curet, and more than 90% of the tumor mass can be quickly removed. The entire surface and border is electrodesiccated or coagulated by slowly drawing the probe back and forth until a uniform char has been created at the base. The charred tissue is removed with the curet, and the desiccation and curettage is repeated two more times or until a normal tissue plane is observed and developed throughout. Desiccating and curetting is continued approximately 0.5 cm beyond the visible borders of the lesion to ensure that microscopic extensions of the tumor are destroyed. Active bleeding from the base may indicate residual tumor. Tumor-free dermis oozes blood in a uniform manner. Bleeding is controlled with Monsel's solution.The wound may be left exposed to the air or may be covered with a bandage or light dressing. Daily washing with soap and water is encouraged. Hydrogen peroxide may be applied once or twice daily; antibiotic ointments are unnecessary. The patient returns in 7 to 10 days, and the adherent crust, if present, is removed. Postoperative care. For large surgical defects that are allowed to heal by secondary intention, infection is prevented and crust formation is discouraged by the following method: The surgical site is painted daily with a thin film of 2% mercurochrome solution with a cotton swab and the skin surrounding the wound is cleaned with hydrogen peroxide and dried thoroughly. The area should be covered with a dry gauze. Bacitracin is used when the wound becomes dry. TECHNIQUES--CURETTAGE Local anesthesia is induced with lidocaine injected with a 27- or 30-gauge needle. Lidocaine can be delivered by jet injector into soft lesions such as warts and seborrheic keratoses. Jet injectors are not usually used on the face. Pencil technique. The pencil technique is best for most soft lesions. Fine, precise movements are possible. The handle of the curet is grasped like a pencil between the thumb and the index and middle fingers. The base of the palm rests on the skin for stability. The skin around the lesion is stretched and held taut by the fingers of the surgeon's free hand. With several smooth, firm strokes the curet is drawn through the tissue. The curet may be pulled toward the surgeon with the index finger or pushed away with the thumb. The surgeon may actually feel the consistency of the tumor with the curet. This is very helpful when curetting nodular basal cell epithelioma, which has a firm, gelatin-like consistency. The dermis at the base of the tumor is very firm and resists curettage. The interface between the tumor and the dermis is not as distinct in elderly patients with actinically damaged dermal connective tissue. Bleeding is controlled with Monsel's solution. |