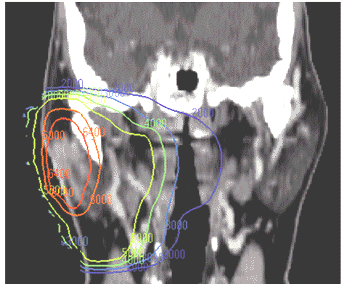
Radiation was delivered through an ipsilateral field of predominantly
high energy electrons in 142 patients (86%). Wedged paired 60Co fields were used to treat
19 patients. The median dose was 60 Gy, typically delivered
at 2 Gy per fraction. The median follow-up time for surviving patients was 155 months.
RESULTS: Forty-seven (29%) patients had disease recurrence, of whom 15 (9%) had disease
recur locally and 10 (6%) regionally (neck). There was no association between the dose of
radiation and local failure, except for a trend for patients with positive margins and/or
named nerve involvement to have improved local control if they received doses > 60 Gy.
There was no difference in failure rates in patients treated with wedged pair techniques
or ipsilateral fields, but there was a higher complication rate in the former. Overall, 37
patients (22%) developed chronic sequelae attributed to radiation. Twelve patients
developed decreased hearing, and 15 patients developed soft tissue or bone necrosis or
exposure. CONCLUSIONS: Local and regional control rates for high
risk patients with parotid gland carcinomas treated with radiation following surgery were
excellent. The technique of using an ipsilateral field encompassing the parotid bed
and treated with high energy electrons often mixed with photons was effective with minimal
severe late toxicity. The moderate complication rate experienced in this series can be
further reduced using modern techniques as described.
 |
The role of post-operative radiation therapy in the treatment of malignant tumors of
the parotid gland.
Imperato JP, Weichselbaum RR, Ervin TJ.
J Surg Oncol 1984
Nov;27(3):163-7
Twenty-nine patients treated with postoperative radiotherapy for malignant tumors of
the parotid gland were reviewed at the Joint Center for Radiation Therapy. Most patients were treated between 5,000 and 6,500 rad. All were
treated because of microscopic residual disease, extra capsular extension, or tumor close
to the facial nerve. The overall results showed one in-field failure, two marginal
recurrences, and eight patients failed distantly. Poor prognostic factors included
high-grade, extracapsular extension, and nodal involvement. We conclude that patients with
malignant tumors of the parotid should be treated with postoperative radiation therapy if
any of the bad prognostic signs are present. This may enable the surgeon to spare the
facial nerve and obtain local control results equal to or better than more radical
surgical procedures.
|
Laryngoscope 1985 Sep;95(9 Pt 1):1059-63
High-grade malignancies of the parotid gland: effective use of planned combined
surgery and irradiation.
Matsuba HM, Thawley SE, Devineni VR, Levine LA, Smith PG
The trend toward treatment of parotid gland malignancies with planned combined surgery
and postoperative radiation therapy is currently being followed by many centers, although
prospective studies confirming the efficacy of this treatment regimen have only recently
begun. We have reviewed only our "high-grade" histologic
types: adenocarcinomas, malignant mixed tumors, high-grade mucoepidermoid carcinomas,
squamous cell carcinomas, and undifferentiated carcinomas. Acinic cell carcinomas,
adenoid cystic carcinomas, and low-grade mucoepidermoid carcinomas were excluded from
study because of their different biologic behavior. Since 1974, we
have employed the approach of surgical extirpation with preservation of the facial nerve
when possible for all parotid tumors, combined with planned postoperative radiation
therapy (50-70 Gy). We reviewed the 37 cases of "high-grade" parotid
gland malignancies and compared the patients treated with the combined modality approach
with our historical patients treated initially with surgery alone. Despite an apparent
higher stage at presentation, our combined treatment group
ultimately had significantly better local control (70% vs. 20%), and an equivalent
survival rate at five years. Tumor was present at the margin of resection in 14
(74%) cases treated with combined surgery and irradiation. The facial nerve was preserved
in six of these patients with positive margins, and only one of these patients developed a
local or regional treatment failure. In conclusion, our data confirms the efficacy of
surgical exploration to determine the extent of disease and surgical resection, preserving
facial nerve function if possible, followed by postoperative radiation therapy at adequate
doses. Control of local-regional disease was much improved by combined modality therapy as
opposed to surgical resection alone, despite the prevalence of residual microscopic
disease in the resection margins. Facial nerve function is optimally preserved by this
approach of conservative surgery combined with postoperative radiation therapy.
Cancer 1993 May 1;71(9):2699-705
Carcinoma of the parotid gland. Analysis of treatment results and patterns of failure
after combined surgery and radiation therapy.
Spiro IJ, Wang CC, Montgomery WW
Department of Radiation Oncology, Massachusetts General Hospital Cancer Center, Boston.
BACKGROUND. The authors retrospectively studied 62 patients with malignant parotid
tumors, treated by combined surgery and radiation therapy between 1975 and 1989. No
patients were lost to follow-up, and all living patients were interviewed. The median
follow-up time was 66 months. RESULTS. Among the 62 patients, there were five isolated
local failures. Distant failure was observed in 11 patients. Neck failure was uncommon
except in patients with advanced neck disease on presentation. The
actuarial 5-year and 10-year local control rates were 95% and 84%, respectively. The
corresponding actuarial disease-free survival (DFS) rates were 77% and 65%, respectively.
Patients with larger tumors, recurrent disease, or involvement of the facial nerve tended
to have lower DFS rates. No statistically significant differences were observed for
patients treated with once-daily versus twice-daily radiation therapy fractionation
schemes. CONCLUSIONS. Treatment was well tolerated, and severe treatment sequelae were
uncommon. In summary, surgery in combination with radiation therapy is highly efficacious
in controlling malignant tumors of the parotid gland.
Clin Oncol (R Coll Radiol) 1995;7(1):16-20
An analysis of radiotherapy in the management of 104 patients with parotid carcinoma.
Sykes AJ, Logue JP, Slevin NJ, Gupta NK
Christie Hospital, Manchester, UK.
A retrospective analysis was made of 104 patients with parotid carcinoma treated with
radical radiotherapy between 1977 and 1986. Eighty-seven patients received postoperative
radiotherapy and 17 had radiotherapy alone. The 5- and 10-year survival figures, corrected
for intercurrent deaths, were 60% and 49% respectively, with primary control rates of 68%
and 58%. Local control was significantly better for patients initially presenting with
T1/T2 disease, but local relapse still occurred in 23% of these patients. Of 13 patients
with acinic cell tumours, four developed local recurrence and a further two had metastatic
disease. These patterns of relapse suggest that patients with parotid carcinoma should
receive postoperative radiotherapy irrespective of disease stage or histological type.
Ann Surg Oncol 1994 Nov;1(6):468-72
Radiotherapy for parotid cancer.
Toonkel LM, Guha S, Foster P, Dembrow V
Department of Radiation Oncology, Mount Sinai Comprehensive Cancer Center, Miami Beach,
Florida 33140.
BACKGROUND: Parotid malignancies represent a heterogeneous group of tumors primarily
managed by surgical extirpation. Moderately high recurrence rates are seen after surgery
alone, and postoperative radiotherapy has been used for patients with higher risks for
local failure. METHODS: To assess the role of radiotherapy in the management of patients
with malignant tumors of the parotid gland, the records of 68 patients receiving
megavoltage therapy at our institution from 1966 to 1989 were reviewed. Patients were
placed into three groups for analyses. Group I was composed of 41 patients receiving
radiotherapy following total gross removal of parotid cancer by surgical procedures,
varying from excisional biopsy through total parotidectomy. Radiation dose for this group
ranged from 4,995 to 6,500 cGy. Group II was composed of 10 patients treated with
radiotherapy after incisional biopsy or excision with positive margins. These patients
received radiation doses of 4,000-9,470 cGy. Group III was composed of 17 patients
receiving radiotherapy for a postsurgical local recurrence. Their radiation dose ranged
from 4,300 to 8,400 cGy. RESULTS: Two of the 41 patients from group I developed a local
recurrence. Two of these patients also developed distant metastases, one concurrent. Two
of 10 group II patients failed locally, whereas three developed distant metastases. Only
nine of the 17 patients in group III were controlled locally, and four patients developed
distant dissemination. CONCLUSION: Total gross excision of parotid
cancer, sparing facial nerve if possible and followed by regional radiotherapy, provides
excellent rates of local control and survival with modest toxicity. Patients
presenting postoperatively with gross residual tumor or recurrence after surgery should be
considered for trials of more aggressive treatment with combined chemotherapy or altered
fractionation schemes of irradiation. |