The
histopathology of axillary skin excised from 12 patients with HS revealed
that ruptured cysts had a lining of stratified squamous epithelium similar
to the epidermis and the epithelium lining hair follicles; there was no
gross dilatation of the apocrine glands The
histopathology of axillary skin excised from 12 patients with HS revealed
that ruptured cysts had a lining of stratified squamous epithelium similar
to the epidermis and the epithelium lining hair follicles; there was no
gross dilatation of the apocrine glands
 A
review of skin biopsies from 101 HS (acne inversa) patients reported
follicular occlusion in all specimens, regardless of disease duration A
review of skin biopsies from 101 HS (acne inversa) patients reported
follicular occlusion in all specimens, regardless of disease duration
 A
study of 51 specimens from 11 patients with HS (acne inversa) noted poral
occlusion, sinus tracts, or cysts; no primary apocrine involvement was
observed. The authors suggest that the homogeneous histopathology of acne
inversa supports its classification as a follicular disease. A
study of 51 specimens from 11 patients with HS (acne inversa) noted poral
occlusion, sinus tracts, or cysts; no primary apocrine involvement was
observed. The authors suggest that the homogeneous histopathology of acne
inversa supports its classification as a follicular disease.
 A
prospective examination of 27 consecutive patients (39 biopsies) found
that the initial lesion was an occluding spongiform
infundibulofolliculitis; stasis and destruction of apocrine glands was a
secondary phenomenon. Similar findings were noted in another study in
which follicular occlusion by keratinous material was a primary event,
with subsequent active folliculitis and secondary destruction of the skin
adnexae and subcutis. A
prospective examination of 27 consecutive patients (39 biopsies) found
that the initial lesion was an occluding spongiform
infundibulofolliculitis; stasis and destruction of apocrine glands was a
secondary phenomenon. Similar findings were noted in another study in
which follicular occlusion by keratinous material was a primary event,
with subsequent active folliculitis and secondary destruction of the skin
adnexae and subcutis.
 HS
is associated with other conditions in which follicular occlusion is a
prominent feature: acne conglobata; pilonidal sinus; and dissecting
cellulitis of the scalp. HS
is associated with other conditions in which follicular occlusion is a
prominent feature: acne conglobata; pilonidal sinus; and dissecting
cellulitis of the scalp.After the
plugging occurs, bacteria invade the apocrine system via the hair
follicles, become trapped beneath the keratinous plugs, and multiply
rapidly in the nourishing environment of apocrine sweat. The glands
subsequently rupture and spread the infection to adjacent apocrine and
eccrine glands, further extending the tissue destruction and skin damage.
The significance of bacterial infection
in HS is controversial. Although bacterial superinfection with
streptococci, staphylococci, and coliforms are considered part of the
pathogenesis of the disorder, cultures from lesions are frequently sterile
and antibiotics are not curative.
Predisposing factors —
Although occlusion of hair follicles may be
a primary event, there may be both acquired and genetic predisposing
factors.
Endocrine —
A
relationship has been proposed between sex hormones and HS. As an example,
HS is seldom seen before puberty, and childhood cases have been associated
with precocious puberty. However, pregnancy and menstruation do not have a
consistent effect on the disease and new onset HS has been reported in
postmenopausal women.
Hyperandrogenism has been suggested as a
causal factor in womem based upon the following observations:
 A
higher free androgen index (due to low serum sex hormone-binding globulin
[SHBG] concentrations) and total serum testosterone concentration in
patients than in normal controls
 Premenstrual
flares have been associated with the androgenic properties of progesterone
and the surge of other ovarian androgens are common. Premenstrual
flares have been associated with the androgenic properties of progesterone
and the surge of other ovarian androgens are common.
 HS
is more prevalent in hirsute women than in weight-matched controls and, in
case reports, has improved after therapy that reduced ovarian and adrenal
androgen production HS
is more prevalent in hirsute women than in weight-matched controls and, in
case reports, has improved after therapy that reduced ovarian and adrenal
androgen production
However, the association between
androgens and HS remains controversial and may be due, in part, to obesity
as many patients with HS are obese and SHBG is negatively correlated with
body mass index A report on the endocrine status of 66 women with HS found
no evidence of biochemical hyperandrogenism when compared to age-, weight-
and hirsute-matched controls Similar findings were noted in another
study. Also arguing against a role for androgens in HS are the
observations that, although acne is more prevalent and severe in males, HS
is predominantly a female disease (13:5), and that HS has been treated
effectively with testosterone in selected patients
HS has been associated with other
endocrine disorders, such as diabetes, Cushing's disease, and acromegaly
Genetic —
There
appears to be a familial predisposition to HS. In one report, a positive
family history of HS was present more often in patients than controls
matched for age and sex (26 versus 2 percent). Other studies examined 62
affected persons (40 females and 22 males) in 11 families. The authors
suggested that HS has a genetic etiology in a pattern consistent with
autosomal dominant inheritance.
Other — HS has
been associated with several cutaneous abnormalities, behaviors, and
nonprescription drugs However, causality has not been proven.
PATHOLOGY — The
histological findings of HS include
 Cystic
epithelium-lined structures containing hair shafts Cystic
epithelium-lined structures containing hair shafts
 Extensive
perifolliculitis Extensive
perifolliculitis
 Spongiform
infundibulofolliculitis Spongiform
infundibulofolliculitis
 Occlusion
of the follicle Occlusion
of the follicle
 Dilatation
of the follicle with stasis in apocrine and exocrine glands
Unlike acne, significant sebaceous gland
involvement is not a component of HS either by histologic examination or
by measuring the sebum excretion rate
Pathologic examination of excised early
lesions demonstrate a local cell –mediated
immune reaction with T-cell lymphocyte predominance. In one series, the
early lesions were associated with a sharp decline in the
T-helper/suppressor ratio in the plasma. However, immunologic studies in
patients with HS have shown mixed results. As an example, systemic cell
mediated immunity and neutrophil function were normal in one report, while
a marked reduction in T-lymphocyte counts was found in another.
CLINICAL MANIFESTATIONS —
The onset of HS is insidious with early
symptoms consisting of pruritus, erythema, and local hyperhidrosis.
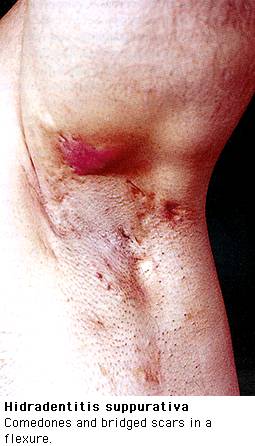
Occlusion of a hair follicle results in a firm, pea-sized nodule or cyst,
similar to the comedones of acne, that can rupture spontaneously and
discharge purulent material. As the area heals, it becomes fibrotic and
new nodules develop adjacent to the original lesions. Some lesions rupture
spontaneously leading to sinus tract formation deep within the cutaneous
tissue; others remain as indurated inflammatory masses. Hyperpigmentation,
scars, and pitting are seen on the skin.
Women have mostly axillary and vulvar
disease, while men are prone to perianal involvement. Single or multiple
cutaneous sites can be affected. The disease may be mild and limited or
severe, with new lesions continually developing and causing chronic,
widespread, deep infection (show figure 1 and show figure 2).
Association with Crohn's disease —
HS and anogenital Crohn's disease are
similar in appearance and may be associated. Minor functional
abnormalities of the gut mucosa or failure of gut IgA to inactivate
bacterial or dietary antigens passing through the small intestine may
result in the formation of IgA immune complexes; these complex may
subsequently be deposited in the skin with resultant disease.
Association with malignancy —
Squamous cell carcinoma arising in HS is
rare, but has been reported in over 16 cases One-half of these patients
died of widespread metastatic disease.
DIAGNOSIS — Early
diagnosis of HS is essential since most cases can be effectively treated
when diagnosed at an early stage. However, specific diagnostic criteria do
not exist. Clinical criteria that suggest early HS include:
 Recurrent
deep boils for more than six months in flexural sites
 Onset
after puberty Onset
after puberty
 Poor
response to conventional antibiotics Poor
response to conventional antibiotics
 Strong
tendency toward relapse and recurrence Strong
tendency toward relapse and recurrence
 Comedones
in apocrine, gland-bearing skin Comedones
in apocrine, gland-bearing skin
 No
pathogens from routine cultures of pus from boils No
pathogens from routine cultures of pus from boils
 Personal
or family history of acne or pilonidal sinuses Personal
or family history of acne or pilonidal sinuses
 Exacerbation
of boils premenstrually in women Exacerbation
of boils premenstrually in women
Late disease is characterized by chronic
infection, draining abscesses, nodules, and scarring. The diagnosis is
based upon characteristic clinical manifestations, biopsy is neither
required nor diagnostic. Cure is unlikely with severe disease extensively
involving a skin site
DIFFERENTIAL DIAGNOSIS —
Only a few processes produce recurrent
abscesses and sinus tract formation with a characteristic distribution in
the apocrine gland-bearing skin.
 Follicular
pyodermas (eg, folliculitis, furuncles, carbuncles, pilonidal cysts) are
also infections arising from a hair follicle. However, they do not result
in the widespread scarring, pitting, and induration observed with HS.
 Granuloma
inguinale causes ulcerations on the vulva or perianal areas, but unlike
HS, may involve the vagina and cervix. Untreated, secondary infection
leading to scarring and tissue destruction can occur. This diagnosis is
established by demonstrating Donovan bodies in scrapings or tissue smears
from the ulcers. Histology shows acanthosis with elongation of the rete
pegs and micro-abscesses. Granuloma
inguinale causes ulcerations on the vulva or perianal areas, but unlike
HS, may involve the vagina and cervix. Untreated, secondary infection
leading to scarring and tissue destruction can occur. This diagnosis is
established by demonstrating Donovan bodies in scrapings or tissue smears
from the ulcers. Histology shows acanthosis with elongation of the rete
pegs and micro-abscesses.
 Perianal
and vulvar manifestations of Crohn's disease include abscesses,
rectoperineal and rectovaginal fistulas, sinus tracts, fenestrations, and
scarring, as well as knife cut ulcers in the inguinal, genitocrural, and
interlabial folds. Differentiation of HS from Crohn's disease depends upon
a previous history of gastrointestinal involvement by the latter but, as
noted above, there may be association between the two disorders. Perianal
and vulvar manifestations of Crohn's disease include abscesses,
rectoperineal and rectovaginal fistulas, sinus tracts, fenestrations, and
scarring, as well as knife cut ulcers in the inguinal, genitocrural, and
interlabial folds. Differentiation of HS from Crohn's disease depends upon
a previous history of gastrointestinal involvement by the latter but, as
noted above, there may be association between the two disorders.
 HS
shares several features with acne: follicular hyperkeratinization leading
to occlusion, fistulous tracts, scarring, and comedome-like lesions.
However, acne is a disease of the sebaceous follicles and sebum
production; it is responsive to medical therapy. By comparison, HS is due
to suppurative inflammation of androgen sensitive terminal hair follicles
with secondary involvement of apocrine, eccrine, and sebaceous glands. It
is a chronic relapsing inflammatory process, poorly responsive to medical
or surgical therapy. Propionibacterium acnes is universally present in
acne lesions, but is not isolated in HS. HS
shares several features with acne: follicular hyperkeratinization leading
to occlusion, fistulous tracts, scarring, and comedome-like lesions.
However, acne is a disease of the sebaceous follicles and sebum
production; it is responsive to medical therapy. By comparison, HS is due
to suppurative inflammation of androgen sensitive terminal hair follicles
with secondary involvement of apocrine, eccrine, and sebaceous glands. It
is a chronic relapsing inflammatory process, poorly responsive to medical
or surgical therapy. Propionibacterium acnes is universally present in
acne lesions, but is not isolated in HS.
MEDICAL
TREATMENT —
Treatment of HS has been difficult
and unsatisfactory in the past. Treatment now is directed at
prevention of new lesions through medical management and elimination of
existing lesions. Medical therapies, including antibiotics, antiandrogens,
and retinoids, have better success in prevention or treatment of early
isolated lesions; established
sinus tracts and extensive lesions of advanced cases respond only to en
bloc surgical excision. There are no data to recommend one medical
treatment over another.
Antibiotics —
Topical clindamycin (1 percent lotion twice per day for three months) is
the only antibiotic that has been shown to be effective in a randomized
placebo-controlled trial extending over a three month period. The number
of abscesses, inflammatory nodules, and pustules was significantly better
than placebo at each monthly evaluation. In another controlled trial,
systemic therapy with tetracyclines (500 mg twice per day for three
months) was as effective as topical clindamycin. Clindamycin also appears
to prevent new lesions after existing disease has been cleared with
isotretinoin and unroofing of sinus tracts.
Antibiotics may diminish odor and reduce
pain, but there is no evidence that long-term antibiotic therapy alters
the natural history of HS. Relapse is almost inevitable after withdrawal
of medication.
Antiandrogens —
Treatment with antiandrogens has produced mixed results in women with HS.
A double-blind controlled, crossover trial comparing ethinyl estradiol (50
mcg) plus cyproterone acetate (50 mg) in a reverse sequential regimen with
ethinyl estradiol (50 mcg) plus norgestrel (500 mcg) (Ovral®) showed that
these treatments were equally effective. After 18 months, 7 of 18 patients
were free of disease, 5 were improved, 4 were unchanged, and 2 worsened.
Patients with infection secondary to extensive hidradenitis responded less
well. Ethinyl estradiol/cyproterone acetate is not approved for use in the
United States.
The author has successfully prevented
recurrent groin and vulvar lesions in five women by discontinuing oral
contraceptive pills with highly androgenic progestins in favor of ethinyl
estradiol/drospirenone (Yasmin), combined with the antiandrogenic action
of spironolactone 50 to 100 mg at bedtime.
Retinoids —
Treatment with low dose isotretinoin (1 mg/kg orally for four months) at
the earliest stages of HS has been used with varying results. As an
example, in one trial of this therapy in 68 patients, the condition
completely cleared during initial therapy in 16 cases and 11 maintained
their improvement during the follow-up period. Treatment is most
successful in the milder forms of HS, possibly by correcting the
follicular abnormality that initiates the processes associated with
chronic disease. The limited therapeutic effect of isotretinoin in HS may
be due to the lack of significant sebaceous gland involvement.
Isotretinoin (2 mg/kg/day in divided
doses) is also a useful adjunctive treatment to reduce inflammation before
and after surgery, but is not effective against epithelial sinus tracts.
Cyclosporine —
Administration of cyclosporine A (4.5 mg/kg per day) has produced moderate
improvement in a few case reports. There are no large trials.
Corticosteroids —
Intralesional corticosteroids have established benefit for patients with
an isolated number of tender lesions, but are not appropriate for
individuals with extensive disease. The lesion is injected with 5 to 10 mg
triamcinolone acetate once monthly for one to three injections.
SURGICAL TREATMENT —
The primary therapy of severe, extensive HS
is surgical. Simple incision and drainage of individual nodules is helpful
to bring short-term relief, but must be followed with active management.
Otherwise, it is almost inevitable that recurrent episodes of inflammation
will occur.
Unroofing — Sinus
and fistulous tracts may be unroofed prior to more definitive surgery or
as part of a multifaceted approach combining medical and surgical
intervention. Under local or regional anesthesia, all tracts are mapped
with a malleable metal probe and then opened with an electrocoagulation
device and scissors. The entire roof of each tract should be completely
removed, the tract curetted, and the epithelialized floor left exposed to
heal by secondary intention. Marsupializing the wound may enhance its
closure. However, there is a high incidence of recurrent disease (over 20
percent), often at a different anatomical site.
Local excision —
Local excision with primary closure has a recurrence rate over 50 percent,
but has a lower morbidity rate than wider ablative en bloc excision.
Wide excision
— Wide excision (margins well beyond the
clinical borders of disease activity) of involved areas is the most
effective treatment of chronic and extensive disease; tissue should be
removed down to soft, normal tissue.
The best method of skin closure is
controversial. Primary closure and rotation flaps are usually not possible
because of the extensive nature of the excision. Grafting in the perineal
and perianal areas is associated with high failure rates. Healing by
secondary intention has shown good results, but wound closure may take
months.
Carbon dioxide laser —
Carbon dioxide laser excision with secondary
intention has been used for mild to severe disease with promising results.
Healing took four to eight weeks and the scars were flat and linear. Only
one recurrence was noted along the margin of the surgical scar in a
previously treated area.
Combined medical-surgical treatment —
For mild to moderate cases, combined
therapies have shown promise in pilot studies. One such regimen consists
of isotretinoin in high doses (2 mg/kg) for six months combined with
surgical therapy: any sinus tracts are unroofed, debrided, and allowed to
heal by granulation. After the course of isotretinoin is completed,
topical clindamycin (2 percent lotion) is applied to prevent recurrent
lesions. Spironolactone (25 mg daily) is then prescribed for its
antiandrogen effect.
TREATMENT SUMMARY —
I try to adhere to the following principles
for the diagnosis and treatment of HS:
 Have
a high index of suspicion for the disease in women with recurrent boils in
apocrine areas after puberty, despite antibiotic therapy. Premenstrual
exacerbation of lesions is also typical of HS.
 Educate
the patient about the course of HS and encourage consistent follow-up to
provide early treatment of lesions. I emphasize the importance of loose
underwear since mechanical friction appears to exacerbate the disease. Educate
the patient about the course of HS and encourage consistent follow-up to
provide early treatment of lesions. I emphasize the importance of loose
underwear since mechanical friction appears to exacerbate the disease.
 For
women with a few isolated lesions without sinus tracts and ongoing
formation of new lesions, I prescribe topical clindamycin (1 percent
lotion twice per day for three months), spironolactone (25 mg daily for
three months), and the oral contraceptive pill ethinyl estradiol
drospirenone (Yasmin) because drospirenone has antiandrogenic effects. I
avoid depot medroxyprogesterone acetate, progestin-only pills and pills
with a highly androgenic progestin. I inject isolated persistent lesions
with triamcinolone. For
women with a few isolated lesions without sinus tracts and ongoing
formation of new lesions, I prescribe topical clindamycin (1 percent
lotion twice per day for three months), spironolactone (25 mg daily for
three months), and the oral contraceptive pill ethinyl estradiol
drospirenone (Yasmin) because drospirenone has antiandrogenic effects. I
avoid depot medroxyprogesterone acetate, progestin-only pills and pills
with a highly androgenic progestin. I inject isolated persistent lesions
with triamcinolone.
 For
women with multiple lesions and sinus tracts, I give isotretinoin (2
mg/kg/day in divided doses) for six months. The sinus tracts should be
unroofed and debrided when the disease remits (ie, no new lesions).
Clindamycin, spironolactone, and oral contraceptive pills can be given for
three months after completion of isotretinoin with follow-up monitoring
every six months. For
women with multiple lesions and sinus tracts, I give isotretinoin (2
mg/kg/day in divided doses) for six months. The sinus tracts should be
unroofed and debrided when the disease remits (ie, no new lesions).
Clindamycin, spironolactone, and oral contraceptive pills can be given for
three months after completion of isotretinoin with follow-up monitoring
every six months.
PROGNOSIS —
The recurrence rate for severe
disease is high even after radical surgery. In a series of 82 such
patients, as an example, the recurrence rate for inguinoperineal disease
was 37 percent. In addition, almost one-quarter of recurrences
developed at a previously unaffected site. |