|
Int J Radiat Oncol Biol Phys 1999 Sep
1;45(2):461-6
Utility of radiation in the prevention of
heterotopic ossification following repair of traumatic acetabular fracture.
Haas ML, Kennedy AS, Copeland CC, Ames JW,
Scarboro M, Slawson RG
Department of Radiation Oncology, University of
Maryland Medical System, Baltimore 21201, USA.
PURPOSE: Heterotopic ossification (HO) is a common
problem following surgical repair of traumatic acetabular fracture (TAF), potentially
causing severe pain and decreased range of motion. This report analyzes the role of
radiation therapy for prevention of HO in TAF. METHODS AND MATERIALS: The charts of all
patients who received RT to the hip following TAF repair between July 1988 and January
1998 were reviewed. Sixty-six patients were identified. RT was given in 5 fractions of 2
Gy in 45 patients, 1 fraction of 8 Gy in 17 patients, and other doses in 4 patients.
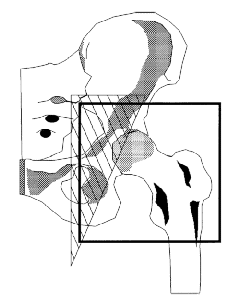
Treatment fields encompassed periacetabular tissues at highest risk for HO. Time to RT was
< or = 24 hours for 46 patients. RESULTS: Radiographic follow-up at least 6 months
following RT was available in 47/66 (71%) patients to permit Brooker classification, revealing 6 cases (13%) of Grade III HO, compared to historical incidence
in this population of 50%. No Grade IV HO was found. Mean follow-up was 18 months.
Four of the Grade III patients had received 10 Gy/5 fractions, and 2 received 8 Gy/1
fraction. Postoperative wound infection occurred in 6 patients, and osteonecrosis of the
femoral head was found in 13. CONCLUSIONS: RT following surgical repair of TAF provides
effective prophylaxis against formation of clinically significant HO. We recommend a single fraction of 7-8 Gy within 24 hours of surgery to
prevent HO formation and minimize patient discomfort.
Int J Radiat Oncol Biol Phys 1998 Jan
1;40(1):171-6
Preoperative vs. postoperative radiation
prophylaxis of heterotopic ossification: a rural community hospital's experience.
Kantorowitz DA, Muff NS
Department of Radiation Oncology, North Puget
Oncology, Sedro-Woolley, WA 98284, USA.
PURPOSE: In vivo data employing a rat model, suggest equivalent suppression of ectopic bone formation by
single-fraction irradiation given either pre (< or = 4 h)- or post (< or = 24
h)-surgery. Two subsequent randomized clinical trials, from tertiary academic
centers with robust experience in heterotopic bone prophylaxis, have reached similar
conclusions. To assess the transferability of the above data to the community setting we
reviewed our rural community hospital experience with pre- and postoperative radiation
prophylaxis. METHODS AND MATERIALS: Between 11/90 and 6/96, 16 surgerized hips with high
risk of heterotopic bone formation received 7.00-8.00 Gy in one
fraction either preoperatively (< or = 4 h) (n = 9) or postoperatively (< or
= 3 days for six hips; day 7 for one hip) (n = 7). Initial patients were routinely treated
postoperatively. In late 1992, treatment preference was switched to preoperative
irradiation in response to evolving data. The two groups were similar with respect to age,
sex, nature of surgery, presurgical Brooker and Harris scores, and in U. of Rochester risk
classification distribution. Irradiation was given via 4-20 MV photons through equally
weighted AP:PA portals to the periacetabular tissues and proximal one third to one-half of
the femoral component. Radiation dose, energy, portal, and blocking design were all
similar for the two groups. Hip radiographs were obtained immediately postsurgery and at
last follow-up: Delta grades (Brooker grade at follow-up--Brooker grade immediately
postsurgery) were computed. Harris scale scores of hip function and movement were assigned
via personal interviews and examinations performed prior to irradiation and at last
follow-up. RESULTS: All 16 hips are evaluable. Follow-up interval among the post-operative
group (mean = 39.8 months; range 18.6-65.8) was significantly longer than among the
preoperative group (mean = 20.4 months; range 8.6-41.3) (p < 0.02). The mean Delta
grade among the postoperative and preoperative groups was identical (-0.02). Similarly,
improvement in Harris scale scores, from preirradiation to last follow-up, were
nonsignificantly different among postoperative (+43.3) and preoperative (+44.8) groups.
There was one postoperative infection in either group; there was no acute or late toxicity
attributable to irradiation. CONCLUSION: As heterotopic bone formation is complete within
6 months, the data for both treatment groups may be considered mature. Our community
generated results parallel those derived from tertiary care centers. Single-fraction
radiation prophylaxis of heterotopic ossification may be given with similar efficacy
either < or = 4 h pre- or < or = 24 h postsurgery. For reasons of minimizing
patient discomfort, postsurgical movement and radiation staff resource utilization, we
prefer and recommend preoperative radiation prophylaxis.
Yonsei Med J 1997 Apr;38(2):96-100
Prevention of heterotopic bone formation after
total hip arthroplasty using 600 rad in single dose in high risk patient.
Han CD, Choi CH, Suh CO
Department of Orthopaedic Surgery, Yonsei
University College of Medicine, Seoul, Korea.
Nineteen patients received single-dose exposure to
600 rad delivered within 48 hours of total hip arthroplasty (THA) with shielding of the
prosthesis region for the prevention of heterotopic ossification. The patients were
considered at high risk for developing heterotopic ossification (HO) because of
hypertropic osteoarthritis, post-traumatic osteoarthritis or the presence of
previously-formed ectopic bone. The average follow-up period was 42 months (range, 37
months-48 months). At a follow-up study, all hips except one were classified as Brooker
class 0. The single exception was classified as class I. All patients were asymptomatic at
the last follow-up study and no component demonstrated subsidence or radiolucent line
indicative of loosening. The authors concluded that 600 rad, single-fraction radiation
therapy is cost effective, convenient and safe for the prevention of heterotopic
ossification after total hip arthroplasty.
Arch Orthop Trauma Surg
1999;119(5-6):296-302
Prevention of heterotopic bone formation after
total hip arthroplasty: a prospective randomised study comparing postoperative radiation
therapy with indomethacin medication.
Kienapfel H, Koller M, Wust A, Sprey C, Merte H,
Engenhart-Cabillic R, Griss P
Department of Orthopaedic Surgery, Philipps
University, Baldingerstrasse, D-35033 Marburg, Germany. kienapfe@mailer.uni-marburg.de
Heterotopic ossification (HO) after total hip
arthroplasty is known to be a major complication with an impact on the functional outcome.
Efforts have been made to prevent the occurrence of HO by means of either radiation
therapy or pharmacotherapy. To date, there are no data available regarding the relative
benefit of radiation versus medication with non-steroidal anti-inflammatory drugs. The
objective of this study was to compare single-dose 600-cGy radiation therapy with
indomethacin medication for their effect on the prevention of heterotopic bone formation
after total hip arthroplasty. In all, 154 patients were included in the study. All
patients underwent primary total hip arthroplasty due to osteoarthritis. Patients were
randomly assigned to three different therapeutic groups. (a) The radiation group received
a single radiation dose of 600 cGy between the 2nd and 4th
postoperative day. (b) The indomethacin group received an oral application of indomethacin
2 x 50 mg per day from the 1st to 42nd postoperative day. (c) The control group received
neither radiation nor indomethacin medication. There were significant group differences (P
< 0.001). A least significant difference test (LSD) revealed that the mean of the
control group was significantly different from that of the radiation and indomethacin
groups. The 13 patients (8.4%) classified Brooker 3 or 4 were all in the control group.
Again, this effect was statistically significant (chi-square, P < 0.001). In
conclusion, this study demonstrated that both radiation and indomethacin therapy are
effective in the prevention of postoperative HO. The choice for either one of the
treatments has to be based on availability, contraindications, side-effects,
practicability, standardisation and cost. Based on these considerations together with the
results of this study, we currently use postoperative radiation with
600 cGy for all patients undergoing primary total hip arthroplasty.
J Bone Joint Surg Am 1992
Feb;74(2):186-200
Prevention of heterotopic ossification with
irradiation after total hip arthroplasty. Radiation therapy with a single dose of eight
hundred centigray administered to a limited field.
Pellegrini VD Jr, Konski AA, Gastel JA, Rubin P,
Evarts CM
University of Rochester School of Medicine and
Dentistry, New York 14642.
Sixty-two hips in fifty-five patients who were
considered to be at risk for postoperative heterotopic ossification were randomly divided
into two groups: one received a single 800-centigray dose of
limited-field radiation and the other, 1000 centigray of limited-field radiation in
divided doses. The risk for heterotopic-bone formation was identified on the basis of
previously described criteria, which included previous heterotopic ossification after an
operation about the hip, hypertrophic osteoarthritis or post-traumatic osteoarthrosis
characterized by formation of extensive osteophytes, radiographic evidence of diffuse
idiopathic skeletal hyperostosis, ankylosing spondylitis, and male sex. The treatment
portals excluded prosthetic surfaces that were intended for biological fixation by
ingrowth of bone. At a minimum six-month follow-up, progression of heterotopic
ossification had occurred in seven (21 per cent) of thirty-four hips in the first group
and in six (21 per cent) of twenty-eight hips in the second group. The ossification had
advanced more than one grade in only one hip. Extra-field ossification occurred in fifteen
(43 per cent) of thirty-five hips that had not had previous heterotopic ossification.
Since the time of the study, the treatment portal has been modified to include the lateral
aspect of the greater trochanter, so that the risk of bursitis associated with
ossification in this area is minimized. Single-dose limited-field radiation is effective
for the prevention of heterotopic ossification, without compromise of early fixation of an
uncemented implant.
Arch Phys Med Rehabil 1995
Mar;76(3):284-6
Heterotopic ossification: treatment of
established bone with radiation therapy.
Schaeffer MA, Sosner J
Department of Rehabilitation Medicine, St.
Vincent's Hospital and Medical Center, New York, NY 10011, USA.
Ectopic bone formation or heterotopic ossification
(HO) is frequently seen on rehabilitation units after total hip arthroplasties, burns, and
neurological injuries. Currently the major role for treatment is in
prophylaxis and the major methods include anti-inflammatory medications, irradiation, and
diphosphanate administration. These prophylactic measures are generally considered to be
ineffective for the treatment of ectopic bone once it has already formed. We
describe two cases of HO for which a radiation therapy protocol was used to treat
established, ectopic bone after it had become problematic. Both patients were found to
have increased range of motion and decreased complaints of pain after treatment, though no
gross plain film x-ray changes were noted. We conclude that
radiation therapy may be useful not only for prophylaxis of heterotopic ossification but
for ectopic bone after it has been formed, especially when pain and progressively
decreased range of motion are problematic.
J Arthroplasty 1998 Dec;13(8):854-9
The suppression of heterotopic ossifications:
radiation versus NSAID therapy--a prospective study.
Sell S, Willms R, Jany R, Esenwein S, Gaissmaier
C, Martini F, Bruhn G, Burkhardsmaier F, Bamberg M, Kusswetter W
Orthopaedic University Clinic Tubingen, Germany.
This prospective, randomized study compares the
effect of postoperative irradiation and nonsteroidal anti-inflammatory drug (NSAID)
therapy on the prevention of heterotopic ossifications after the implantation of a total
hip endoprosthesis. A total of 154 operations were performed; one group of patients
underwent radiation treatment of 3 x 3.3 Gy, and the other group took 3 x 50 mg of
diclofenac per day over a period of 3 weeks. Average age, sex, preoperative diagnosis, and
risk factors were similar in both groups. Postoperative radiation began on average 2.9
days after operation, and the radiation therapy was finished on average within 3.8 days.
NSAID prophylaxis was begun on the first postoperative day. Heterotopic ossifications
occurred in two of the patients who had undergone postoperative prophylaxis by radiation.
In both cases, the ossification was Brooker I, and there was no functional impairment.
There were no ossifications of Brooker II-IV in this group. One patient had a
Staphylococcus epidermidis infection, and fistula revision had to be carried out; the
prosthesis could be left in place. In the group treated with NSAID, 16 heterotopic
ossifications stage Brooker I and 2 stage Brooker II could be detected. Eleven patients
stopped the treatment because of gastrointestinal problems. Both postoperative radiation
and NSAID therapy have proved to be effective prophylactic methods. In
direct comparison, radiation prophylaxis by 3 x 3.3 Gy proved to be slightly more
successful than NSAID prophylaxis.
Complications of total hip arthroplasty
Heterotopic ossification —
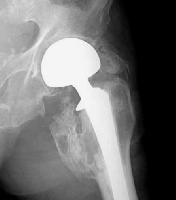
Heterotopic ossification (HO) is a process by
which the soft tissues around the hip become ossified. Following total hip
arthroplasty, HO typically occurs around the femoral neck and adjacent to
the greater trochanter. HO occurs when primitive mesenchymal cells in the
surrounding soft tissues are transformed into osteoblastic tissue. This
tissue then forms mature lamellar bone.
Incidence —
The
incidence of HO varies widely and may reach up to 90 percent when evaluated
in high risk populations.
Risk factors for HO —
The exact trigger for HO following total hip
arthroplasty is unknown, but risk factors have been identified.
 HO
is twice as common in males as compared to females.
 Patients
at high risk for developing HO after total hip arthroplasty include men with
bilateral hypertrophic osteoarthritis, patients with a history of HO in
either hip, and patients with posttraumatic arthritis characterized by
hypertrophic osteophytosis. Patients
at high risk for developing HO after total hip arthroplasty include men with
bilateral hypertrophic osteoarthritis, patients with a history of HO in
either hip, and patients with posttraumatic arthritis characterized by
hypertrophic osteophytosis.
 Patients
at moderate risk include those with ankylosing spondylitis, diffuse
idiopathic skeletal hyperostosis (DISH), Paget's disease, or unilateral
hypertrophic osteoarthritis. Patients
at moderate risk include those with ankylosing spondylitis, diffuse
idiopathic skeletal hyperostosis (DISH), Paget's disease, or unilateral
hypertrophic osteoarthritis.
 Other
risk factors include females over the age of 65 at the time of surgery, and
a lateral surgical approach to the hip. Although one study by Maloney found
that the incidence of HO was higher with cementless femoral components, more
recent studies have shown that type of fixation (cemented or cementless)
does not affect the incidence of HO Other
risk factors include females over the age of 65 at the time of surgery, and
a lateral surgical approach to the hip. Although one study by Maloney found
that the incidence of HO was higher with cementless femoral components, more
recent studies have shown that type of fixation (cemented or cementless)
does not affect the incidence of HO
Symptoms —
Hip
stiffness is the most common complaint. Pain is rarely a problem. Many
patients with radiographically low-grade HO are asymptomatic
Physical findings —
Some patients with severe HO may have signs of
inflammation including fever, erythema, swelling, warmth, and tenderness.
Such findings are also suggestive of wound or prosthetic joint infection.
Laboratory studies —
Development of severe HO has been correlated
with a sedimentation rate greater than 35 mm/hr and a serum alkaline
phosphatase greater than 250 IU/L at 12 weeks postoperatively.
Classification —
HO is typically evaluated radiographically. The most widely accepted
classification system includes four grades based on an AP radiograph of the
pelvis and hip
 Grade
I represents islands of bone within soft tissues about the hip.
 Grade
II includes bone spurs adjacent to the pelvis or proximal end of the femur
leaving at least 1 cm between opposing bone surfaces. Grade
II includes bone spurs adjacent to the pelvis or proximal end of the femur
leaving at least 1 cm between opposing bone surfaces.
 Grade
III represents bone spurs adjacent to the pelvis or proximal end of the
femur leaving less than 1 cm between opposing bone surfaces Grade
III represents bone spurs adjacent to the pelvis or proximal end of the
femur leaving less than 1 cm between opposing bone surfaces
•Grade IV represents radiographic
ankylosis of the hip.
Imaging —
Findings of ossification may be visible on plain radiographs within 3 to 4
weeks postoperatively. Maturation of the HO may take up to 1 or 2 years.
Bone scanning typically shows increased uptake in the soft tissues adjacent
to the hip. But these findings are not specific for HO.
The maturation process can be monitored by
serial radiographs or bone scan.
Prophylaxis for
HO —
The first step in
effective prophylaxis is to identify patients who are at high risk for HO
preoperatively. Routine use of prophylaxis is not indicated. Currently,
nonsteroidal antiinflammatory drugs (NSAIDs) and external beam radiation
have been used most successfully in preventing HO. Prophylactic measures
against HO after total hip arthroplasty should be administered before the
fifth postoperative day, optimally within 24 to 48 hours.
 Indomethacin
— Indomethacin is the most commonly
used NSAID for HO prophylaxis, although other NSAIDs have demonstrated some
effectiveness. Selective COX-2 inhibitors, unlike traditional NSAIDs, have
not demonstrated effective HO prophylaxis. The recommended dose of
indomethacin is 75 to 100 mg/day and should be continued for 7 to 14 days
postoperatively. Bleeding complications are more frequent in patients
receiving indomethacin in conjunction with anticoagulation for
thromboembolic prophylaxis, and careful monitoring should be implemented.
 External
beam radiation
— External beam
radiation has also demonstrated efficacy in prevention of HO after total hip
arthroplasty. A year 2004 meta-analysis of seven randomized studies that
compared radiation to NSAIDs
concluded that radiotherapy is more effective, but the absolute
difference in the rates of clinically significant HO are quite small, on the
order of one percent. A single dose
regimen of 700 or 800 centigray is recommended.
Radiation may be administered
preoperatively (within 24 hours) or postoperatively (within 72 hours). If
cementless prosthetic components are used, the ingrowth areas should be
shielded from the radiation beam. Currently, there is no clinical
evidence supporting malignant transformation following this type of single
dose regimen. External
beam radiation
— External beam
radiation has also demonstrated efficacy in prevention of HO after total hip
arthroplasty. A year 2004 meta-analysis of seven randomized studies that
compared radiation to NSAIDs
concluded that radiotherapy is more effective, but the absolute
difference in the rates of clinically significant HO are quite small, on the
order of one percent. A single dose
regimen of 700 or 800 centigray is recommended.
Radiation may be administered
preoperatively (within 24 hours) or postoperatively (within 72 hours). If
cementless prosthetic components are used, the ingrowth areas should be
shielded from the radiation beam. Currently, there is no clinical
evidence supporting malignant transformation following this type of single
dose regimen. |