|
Is
there a dose-effect relationship for the treatment of symptomatic
vertebral hemangioma?
Rades. IJROBP; 2003:55:178
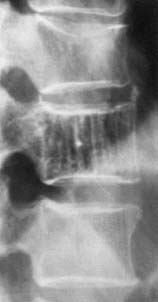
Radiologic
examinations contribute to the diagnosis. On plain X-ray films, the
so-called “honeycomb” appearance or coarse vertical striations can be
observed, if at least one-third of the vertebral body is involved.
Sometimes compression fractures can be seen. The CT scans may show the
so-called “polka dot” appearance representing axial cuts caused by
thickened vertical trabeculae. MR imaging is helpful for the
differentiation between intraosseous (nonevolutive) and extraosseous (more
frequently associated with symptomatic lesions)
hemangioma. Because of a
higher content of fat tissue, intraosseous lesions show an increased
signal on T1- and T2-weighted images. Extraosseous lesions contain only
little fat and show an isointense signal on T1- and an increased signal on
T2-weighted images.
Symptomatic vertebral
hemangiomas are rare. Onset of symptoms most frequently occurs in the
fourth or fifth decade of life. The relation of female to male ranges
between 2:1 and 9:2 . The symptom most frequently observed is pain, but
motor dysfunction due to spinal cord compression may also occur.
Therapeutic
intervention is indicated only if relevant symptoms develop. Radiotherapy
(RT) is the most common treatment for painful lesions. Other conservative
treatment options are embolization, intralesional injection of ethanol, or
vertebroplasty with methyl methacrylate Surgery is often performed in the
case of spinal cord compression. This analysis was performed to
investigate a possible dose-effect relationship and to enable a
recommendation for the total radiation dose to be applied.
 :
Individual data from our own and published patients with symptomatic
vertebral hemangioma treated
with radiotherapy alone were obtained. The data were pooled, and the
impact of the total dose on complete pain relief was evaluated using the
chi-square test. Because different single-fraction doses were used, the
equivalent dose in 2-Gy fractions (EQD2)
was used for the analysis. :
Individual data from our own and published patients with symptomatic
vertebral hemangioma treated
with radiotherapy alone were obtained. The data were pooled, and the
impact of the total dose on complete pain relief was evaluated using the
chi-square test. Because different single-fraction doses were used, the
equivalent dose in 2-Gy fractions (EQD2)
was used for the analysis.
 :
Complete data could be obtained from 117 patients. Patients were
categorized according to total dose (EQD2)
into two groups of similar size
(Group A: 20–34 Gy, n = 62; and Group
B: 36–44 Gy, n = 55).
Radiation-induced complete pain relief was achieved in 39% (24/62) of the
patients in Group A and in 82% (45/55) of the patients in Group B.
The difference was statistically significant (p
= 0.003). :
Complete data could be obtained from 117 patients. Patients were
categorized according to total dose (EQD2)
into two groups of similar size
(Group A: 20–34 Gy, n = 62; and Group
B: 36–44 Gy, n = 55).
Radiation-induced complete pain relief was achieved in 39% (24/62) of the
patients in Group A and in 82% (45/55) of the patients in Group B.
The difference was statistically significant (p
= 0.003).
 :
The data suggest a dose-effect relationship in the radiotherapy of
symptomatic vertebral hemangiomas.
We recommend a total radiation dose 36–40 Gy with a dose per fraction of
2.0 Gy. :
The data suggest a dose-effect relationship in the radiotherapy of
symptomatic vertebral hemangiomas.
We recommend a total radiation dose 36–40 Gy with a dose per fraction of
2.0 Gy.
Radiotherapy is effective in the treatment of symptomatic vertebral
hemangiomas (SVH): Long-term results of a multicenter study in germany
Micke. 2004;60:S244
Vertebral
hemangioma is the most
commonly encountered tumor of the vertebral column with an estimated
incidence of 10–12% in the western population. Only 0.9–1.2% of all
vertebral hemangiomas are symptomatic with pain as main complaint
requiring treatment. The use of radiotherapy (RT) in SVH has a long
tradition, but optimal dose and possible late effects are controversial
in the light of new treatment options, like microsurgery and
vertebroplasty.
Materials/Methods
Seven cooperating
German institutions collected clinical features, treatment concepts, and
outcome data of all patients with SVH referred to local RT during the
last 35 years; the updated outcome was determined from case history
notes, tumor registry correspondence or by individual telephone
interviews. Study end points were pain relief after RT (complete,
partial, or no pain relief), symptomatic and radiological response,
recurrent disease activity, and treatment-related side effects. Median
follow-up time was 68 (6–422) months.For comparison a comprehensive
literature review with 65 published studies (1929–2003) representing 355
patients was used.
Results
From 1969 to 2003 a
total of 82 patients with 86 lesions were irradiated for SVH. There were
56 female and 26 male patients (gender ratio: 2.2:1). Diagnosis was
primarily radiologically confirmed, 18 patients (22.0%) had additional
biopsy confirmation. Median age was 48 (12–79) years. Thoracic spine was
most often involved (n = 45; 55.8%), followed by lumbar (n = 35; 42.7%),
and cervical spine (n = 2; 2.5%). Primary symptom for treatment
indication was pain, 23 (28.0%) patients had additional neurological
symptoms. In most patients one vertebral body was involved, 11 (13.4%)
had one or more involved vertebrae. Prior to RT, 19 Patients (23.2%) had
a surgical intervention.
Radiotherapy of the
involved bony and soft tissue structures was performed with a median
total dose of 34 (4.5–45) Gy, the median single dose was 2 (0.5–3) Gy.
RT was carried out with linacs in 48.8% (n = 40), Co-60 units in 41.5%
(n = 34), and orthovoltage units in 9.7% (n = 8).
A total of 61% of patients
reached complete and 29.2% partial symptomatic remission, only in 9.8%
no pain remission was achieved. 8 patients had recurrent symptoms
after a median time of 70 months, resulting in a
long-term control rate of
90%. In 27% radiological signs of reossification were
observed. However, logistic regression showed no significant correlation
with pain relief. Age, gender and tumor location also revealed no
significant influence on pain response. Most important, however,
total doses of 34 Gy and above
had significantly superior treatment results and fewer recurrences than
total doses lower than 34 Gy.
No acute and late
radiogenic side effects >Grade 2 (RTOG/EORTC) were observed, and
particularly no secondary malignancies.
In comparison, the
literature review revealed a
slightly lower complete response rate with a mean of 58%.
Conclusions
This study comprises
the largest data base of cases reported for RT in SVH. RT is an easy,
save and effective method of pain-relief treatment for SVH. Total doses
of at least 34 Gy give better symptomatic response, but without
correlation to radiological response. The study may serve as a starting
point for a patterns of care study on RT for SVH. An (inter-) national
registry for rare benign diseases is recommended to include this benign
disorder
|