|
|
Is Radiation Plus Chemotherapy as Good
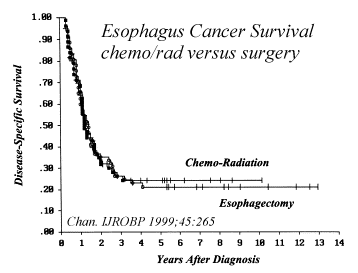
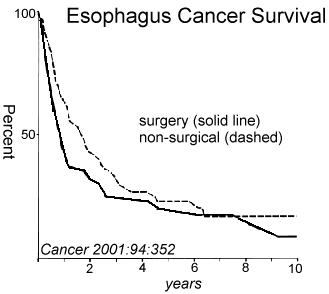
as Surgery? Radiation alone has such a poor cure rate for esophagus cancer that many studies have evaluated combining radiation with chemotherapy which improves the cure rates. Some studies have compared chemo/radiation with surgery and found the results similar, suggesting that surgery may not be necessary. A recent study (Chan. IJROBP 1999;45:265) compared chemotherapy (Mitomycin/ 5FU/ leukovorin) plus Radiation (50-60Gy) and had survival rates by stage: stage I 55%/5y, stage II 16%/5y and stage III 8%/5y. The overall results with chemoradiation (25%/5y survival) were the same as those patients treated with surgery (23%/5y survival.) Other studies are noted below: |