Nonsmall
cell lung cancer presenting with synchronous solitary brain metastasis,
Hu, M. D. Anderson Cancer Center, Cancer 2006;106:1998
The
optimal treatment for the primary
site in patients with newly diagnosed NSCLC who have solitary brain
metastases is not well defined, although several studies have shown
that some patients might benefit from aggressive therapy. We sought to
distinguish which patients with solitary brain metastases treated with
surgery or SRS might benefit from aggressive treatment of their primary lung
cancer.
The cases of 84 newly diagnosed NSCLC patients presenting with a solitary
brain metastasis and treated from December 1993 through June 2004 were
retrospectively reviewed at The University of Texas M. D. Anderson Cancer
Center. All patients had undergone either craniotomy (n = 53) or SRS (n =
31) for management of the solitary brain metastasis. Forty-four patients
received treatment of their primary lung cancer using thoracic radiation
therapy (median dose 45 Gy; n = 8), chemotherapy (n = 23), or both (n = 13).
The median Karnofsky performance status score was 80 (range, 60-100).
Excluding the presence of the brain metastasis, 12 patients had AJCC Stage I
primary cancer, 27 had Stage II disease, and 45 had Stage III disease. The
median follow-up was 9.7 months (range, 1-86 months). The 1-, 2-, 3-, and
5-year overall survival rates from time of lung cancer diagnosis were 49.8%,
16.3%, 12.7%, and 7.6%, respectively.
The median survival times for
patients by thoracic stage (I, II, and III) were 25.6, 9.5, and 9.9 months,
respectively (P = .006).
By applying American Joint Committee on Cancer staging to only the primary
site, the thoracic Stage I patients in our study with solitary brain
metastases had a more favorable outcome than would be expected and was
comparable to Stage I NSCLC without brain metastases.
Aggressive treatment to the lung may
be justified for newly diagnosed thoracic Stage I NSCLC patients with a
solitary brain metastasis, but not for locally advanced NSCLC patients with
a solitary brain metastasis.
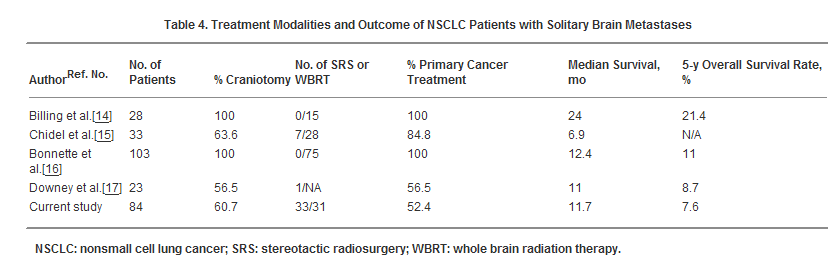
Billing studied 28 patients with brain metastases from NSCLC who underwent craniotomy and resection of the lung primary tumor. Seventeen patients had N0 disease, 5 had N1 disease, and 6 had N2 disease. The 5-year survival rate for patients with N0 disease was 35% compared with 0% in patients with N1 or N2 lymph node disease. Negative lymph nodes appear to be an important prognostic factor for patients even in the presence of a single brain metastasis. Bonnette observed median survival durations of 12.4 months in 103 patients treated with surgery for both the primary tumor and brain metastases, with a 5-year survival overall rate of 11%. We compared the current study group of patients with our database of 1002 lung cancer patients treated in the Department of Radiation Oncology at M. D. Anderson. The overall survival rate for patients with synchronous solitary brain metastasis was worse than that of the whole database (P<.01). But for the Stage I patients with synchronous brain metastases, there were no significant differences between the 2 groups of patients with or without brain metastases, , and the result was similar to Mountain However, there were significant differences of survival rates for Stage II and III patients between patients with or without brain metastases Also, there were significant differences of overall survival rate and chest control for Stage I patients compared with Stage II and III (53% vs. 24%). The data suggest that aggressive treatment of both the brain metastases and primary NSCLC is indicated for thoracic Stage I patients.
|
|
|
|
|
|