Cancer of the appendix is an
uncommon disease that is rarely suspected rarely before surgery. Although several case
series of these tumors have been published, little research has been anchored in
population-based data on cancer of the appendix.
METHODS
This analysis included all actively followed cases of appendiceal neoplasms reported to
the National Cancer Institute's Surveillance, Epidemiology and End-Results (SEER) program
between 1973 and 1998. Tumors were classified as colonic type adenocarcinoma, mucinous
adenocarcinoma, signet ring cell carcinoma, goblet cell carcinoid, and malignant carcinoid
(SEER only collects data on carcinoids specifically classified as malignant). We compared
incidence, overall survival and survival rates by extent of disease at diagnosis.
RESULTS
From 1973 to 1998, 2117 primary malignant tumors of the appendix were reported to the SEER
program. Adenocarcinomas were more likely to be excluded due to a previous diagnosis of
malignancy (9% vs. 3-4% for the other histologies). No other differences in proportions of
cases excluded were identified. There were 1689 cases eligible for inclusion in the study,
1645 of which were analyzed for the five most common histologic tumor types.
The age-adjusted incidence of appendiceal malignancies in the population represented by
the SEER program was 0.12 cases per 1,000,000 people per year (crude incidence 0.12 cases
per 1,000,000 people per year). No temporal trends in incidence were noted over the
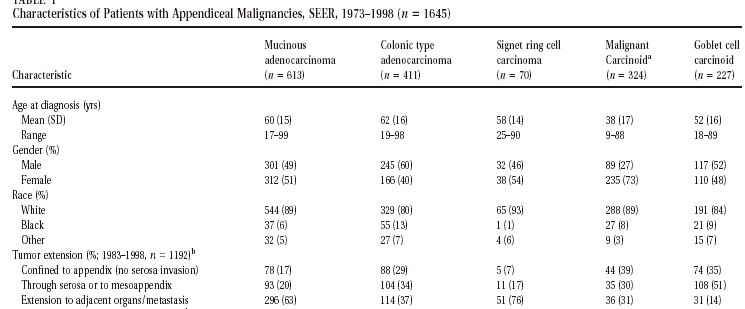
26-year period. Table 1 shows patient characteristics for 1645 tumors in each of the five
most common histologic types. Mucinous adenocarcinoma was the most frequent diagnosis,
with 613 cases (37% of total). After controlling for age and extent of disease at
diagnosis, the overall survival rate for patients diagnosed between 1983 and 1997 (n =
1061) was significantly worse for those with signet ring cell carcinoma than for those
with any other tumor type (P < 0.01). In addition, overall survival rates were better
for patients with malignant carcinoid (P = 0.01). Except for signet ring cell carcinoma
and malignant carcinoid, histology did not have a significant impact on survival when age
and extent of disease at the time of diagnosis were taken into account. Even though the
unadjusted data suggest that a difference in survival does exist among the other tumor
types, much of the difference in these data is explained by the degree of disease spread
that is present when the tumors are discovered. Survival analysis by extent of disease
limited the number of cases that were analyzed because detailed data on tumor spread were
not collected before 1983. Therefore, the subsets within each group were small (Table 1).
Future analyses of population-based data that include more cases may detect differences in
survival between the other histologies. Alternatively, no other differences in survival
may be present between the histologies.
The data analyzed for this population-based study confirm many of the findings reported
from smaller case series of appendiceal malignancies. As suggested by other authors, the
overall biologic behavior of goblet cell carcinoids in our series was intermediate between
that of adenocarcinomas and carcinoid tumors in terms of age at diagnosis, extent of
disease spread at diagnosis, and number of cases with lymph node involvement.[17][18]
The contrast between mucinous adenocarcinoma and the so-called colonic type adenocarcinoma
of the appendix has been given much consideration.[18][19] The tumors are separate
entities and the survival for patients with mucinous adenocarcinoma is better than that of
people with the nonmucinous variety in two studies and worse in one.[5][7][18] In our
study, the hazards of death were equivalent for mucinous adenocarcinoma and colonic type
adenocarcinoma. Although no differences in survival were evident, the differences in
gender ratio and affected ethnicities support the notion that mucinous adenocarcinoma and
colonic type adenocarcinoma are two distinct morphologies.
Primary signet ring cell carcinoma of the appendix is an exceedingly rare entity, and
little information on the distinct characteristics of this tumor has been published. Like
signet ring cell carcinomas of the stomach and colon, people with signet ring cell
carcinoma of the appendix in this study had greater tumor extension at the time of
diagnosis. Survival for patients with this type of tumor in the appendix is significantly
worse than for patients with other tumor histologies.[10] Moreover, the signet ring cell
morphology itself did adversely affect survival even after disease extent and age were
taken into account. Signet ring cell carcinoma is likewise a distinct tumor type in the
appendix that should be considered separately from other carcinomas, especially because of
its poor prognosis.
As has been described for carcinoid tumors in general, malignant carcinoids in this
analysis were more common in women, had a younger average age at diagnosis, and had a
better overall survival than all other histologic types of appendiceal tumors.[20][21]
Malignant carcinoid was the only other histology that had an impact on survival
independent of age and extent of disease at time of diagnosis.
The data used for this study were collected from many sites around the United States and
include diagnoses from hundreds of pathologists. Because of the way in which the data were
collected, there are no effective means of establishing the reliability of the tissue
diagnoses. Some of the diagnoses submitted to the SEER program may be incorrect, which
could impact the reliability of our results. Our findings from this large-scale analysis
confirm many of the findings already reported in the literature about appendiceal cancers.
Even though our conclusions are limited by the observational nature of this study, these
data may serve as a basis for comparison for future studies.
This study is the most extensive comparison of tumors of the appendix by histology
published to date. The use of population-based data enhances the generalizability of the
findings by including cases reported from a variety of institutions within a defined
population. Surveillance data offer a statistically robust yet systematic view of
appendiceal cancer, revealing information about the relative importance of histology and
extent of disease that can help physicians and their patients to understand the
implications of the diagnosis. |